I. Symptoms of C Diff
II. Cause of C Diff
III. C Diff Diagnosis
IV. Standard Medical Treatments of C Diff
V. What is the Best Diet for C Diff?
VI. New Treatments Currently Being Studied
VII. Non-Conventional Treatments for D Diff
VIII. Probably Bad for C diff
IX. Either Good or Bad for C Diff
X. Things That Probably Have No Effect
XI. Ideas to Manage Anxiety
XII. Things To be Cautious About
XIII. Success Stories
XIV. Frequently Asked Questions
I. WHAT ARE THE SYMPTOMS OF C-DIFF. (CLOSTRIDIODES DIFFICILE)?


The symptoms of C. Diff can vary substantially.
Typical symptoms are mild abdominal pain and diarrhea
with or without mucous.
However, some people also report experiencing
nausea, vomiting and severe abdominal pain.
In contrast, a minority of people report never experiencing
diarrhea or mucus.
Symptoms typically begins 5 to 10 days after starting antibiotics—
but may occur on the first day of antibiotics, or up to 2 months after
finishing antibiotics. But, it should be pointed out,
that some people get
c diff without ever taking antibiotics.
In the worst case of c diff, patients may have abdominal pain, nausea, vomiting,
and diarrhea, which results in the person not only having c diff, but also
having dehydration.
These symptom may require them to be admitted to a hospital for treatment.
However, most people who have c diff can receive oral antibiotics
and be treated at home.
II. WHAT IS THE CAUSE OF C. DIFF. (CLOSTRIDIODES DIFFICILE)?
C. Diff is caused by a baterium, which is now called Clostridioides D.
(klos-TRID-e-OY-dees dif-uh-SEEL).
Its name was changed in 2016 because its bilological analysis
showed that it more correctly belonged to the clostridiodes genus--
rather than the clostridium genus.
This bacterium can be a part a person’s normal intestinal
flora or it can be transmitted from one person to another.
Approximately 40% of infants have clostridiodes at birth,
and up 15% of adults clostridiodes dificile without having any
symptoms.
A second way to get c diff is for a person to swallow
some C. diff spores either in food or by touching objects
contaminated with C. diff spores and then putting
their fingers in their mouth. Often times, it difficult
to determine how C. diff was transmitted to a person.
Sometime after the C diff spores are a person's
intestines a favorable environment occurs, which allows
the C. diff spores to grow (germinate) into a toxin
producing bacterium. The toxins produced then cause
damage to the host colon, which in turns causes
symptoms such as nausea and diarrhea.
Typically, C. diff. infection occurs when a person is
given strong intravenous antibiotics, which kill
a lot of the colon's good bacteria. This in turn
allows the C. diff spores to become C. diff bacteria.
While this usually occurs as a result of very powerful
intravenous antibiotics, it can also occur as a result
of mild oral antiobitics, or to chemotherapy. It can
also occur without any no cause.
III. HOW IS C. DIFF. DIAGNOSED?
C. Diff. can be diagnosed by a careful history and tests of the stool.
There are 4 different tests for c diff. Unfortunately, none of these are
100% accurate. Also, unfortunately, different doctors will order different
c diff test.
1. Cytotoxin Assay (~90% accurate)
2. PCR (or NAA Test) toxin A & B "gene" test (~99% accurate)
3. [EIA] ELISA C diff toxin test (~75% accurate)
4. [EIA] ELISA GDH Enzyme Antigen test (~90% accurate)
The Cytotoxin Assay is the most expensive and rarely done because of expense.
It also has a chance of a false positive. Basically, a stool sample is placed on a thin
layer of human foreskin and watched for a reaction.
The PCR (Polymerase Chain Reaction) test is a type of NAA Nucleic Acid Amplification test.
This test looks for one or two genes that are present in a toxin produced by c diff. This
is a very sensitive test for genes, but the presence of these genes does NOT
determine if c diff bacteria are currently producing active toxins. Therefore, this
test is usually a very good test for someone who has never had c diff, but if a person has had
a c diff infection within the last 3 months, it can give a false positive.
The ELISA (Enzyme Linked Immmuosorbent Assay) c diff test basically takes a watery stool
sample and adds a preprepared antibody to the solution. If there is a reaction between
the bacteria in the stool and the preprepared antibody, the test is considered positive.
This test rarely has false positives, but because the c diff bacteria can die very quickly
when it is exposed to air, it can have a high number of false negatives (approximately 25%).
The ELISA GDH Antigen test is similar to the ELISA c diff test, but instead of looking for
a reaction between the bacteria and the preprepared antibody, it looks for a reaction between
the GDH Antigen Enzyme (which can be secreted by any bacteria in the colon--including c diff)
and another preprepared antibody. This is a very sensitive test (approximately 90%),
and is usually accurate for
c diff, but CAN be positive due to another bacterium in the colon.
Basically, since none of these c diff tests are 100% accurate,
oftentimes several tests are used to make the diagnosis of c diff.
Reference: Understanding C Diff Tests Reference
Reference: Sensitivity of C Diff Tests Reference
IV. WHAT ARE THE STANDARD MEDICAL TREATMENTS FOR C. DIFF.?
1. Oral Antibiotics:
A. Oral Vancomycin: usually 125 mg 4 x /day for 10 days. (Sometimes longer,
Sometimes higher doses)
 B. Fidaxomycin (Dificid) 200 mg tablet 2 x /day for 10 days
B. Fidaxomycin (Dificid) 200 mg tablet 2 x /day for 10 days
(Sometimes repeat treatments
are required, and the repeat treatment can be a tapered dose.
C. Both vancomycin and fidaxomycin can be prescribed to prevent a relapse of c diff in people
who are at a high risk for a relapse. The doses are usually one to two pills per day for the
time a person is on another antibiotic plus 5 to 7 days more.
Reference: American College of Gastroenterology
2. Antidiarrheal agents:
 A. Bismuth Subsalicylate (BSS) (Pepto Bismol) - has antibacterial properties against C. Diff. ;
therefore,
might be of some benefit in treating C. Diff.
A. Bismuth Subsalicylate (BSS) (Pepto Bismol) - has antibacterial properties against C. Diff. ;
therefore,
might be of some benefit in treating C. Diff.
Reference: Pepto Bismol
B. INITIALLY, Imodium and Lomotil are not recommended to treat C. Diff. because they
have no anti C. Diff.
qualities and may indirectly increase the toxins that affect the large intestine.
However, they can sometimes be used after c diff antibiotics are started.
However, they must be used judiciously
to avoid causing constipation or interfering with the desired actions of the c. diff
antibiotics.
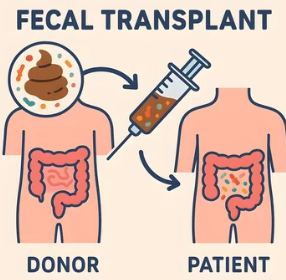 3. Fecal Microbial Transplant (FMT):
3. Fecal Microbial Transplant (FMT):
A. FMT via a colonoscopy (~91% cure rate)
B. FMT via a nasal gastric tube (~81% cure rate
C. FMT via pills (Vowst) FDA approved in 2024 (~96% cure rate)
D. FMT via enema (Rebyota) (~83% cure rate)
V. What is the Best Diet for C Diff?

DON'TS
1. Don't Eat a High-Protein Diet
2. Don't Eat a High-Fat Diet
3. Don't Drink Protein Drinks or Shakes
4. Don't Eat a High-Calcium Diet
5. Don't Eat a High-Sugar Diet
6. Don't Eat a Lot of Salt
7. Don't Drink a lot of Alcohol
DOs
Some foods of food groups that you should probably eat or drink.
1. Do Consider a Low FODMAP Diet
2. Do Consider an Elimination Diet
3. Do Consider Eating Some Formented Foods
4. Do Consider Eating Some High-FODMAP Foods
3. Do Consider Eating Some Fruits
6. Do Drink SUFFICIENT Water
1. Don't Eat a Lot of Protein
There was a study of two groups of mice fed a relatively similar
diets but the diets differed in the amount of protein and
fat. Diet 5010 contained approximately 24% protein and 10% fat
and, and Diet 5053 contained approximately 20% protein and 5% fat.
Both groups of mice were infected with c diff, but the group
that were fed Diet 5053 (20% protein and 5% fat diet) had less colon
inflammation (colitis).
REFERENCE:
Lower
Protein and Fat Diet decreases C diff Severity
A second reason that protein consumption is probably not a good idea
is that a second mice study found that reducing glycine among hamsters
reduced their rate of dying. (Glycine is a type of protein that is found
in most types of animals (meat, foul, and fish) and to a lesser extent
in many types of beans.
This study is more complicated than simply not feeding hamsters
glycine, instead the researchres
created a type of c diff bacteria that was unable
to digest glycine. The researchers just infected hamsters with
their created bacteria versus a group of hamsters infected with the
average c diff bacteria. The hamsters given the created c diff
lived longer before dying than the other hamsters.
REFERENCE:
Glycine Reducation Diet Reduces C Diff among Infected Hamsters
A third study also found a correlation between a high-animal protein
diet (meat) and decreased levels of
Eubacterium Rectale and Roseburia Intinalis Bacteria.
Both of these bacteria
produce butyrate, and butyrate reduces inflammation. Therefore,
these bacteria are considered good gut bacteria.
REFERENCE:
High-Animal-Protein Diet is Correlated with Inflammatory Bowed Disease Reference
In reality, it is nearly impossible to avoid all protein and it
would not be healthy for a person to avoid
all protein for a long period of time;
however, it is possible to decrease the amount of protein
eaten for a short period of time
in the hopes that it might
decrease the chance of c diff relapse.
REFERENCE: High Red Meat Consumption is Correlated with Cancer,
Heart Disase, and Kidney Disease Referenc
2. Don't Drink Protein Supplements
A study tested 17 different
sources of protein in protein drinks and found that NONE of them
were beneficial to the colon.
Although protein supplements might sound like a logical way to help
the intestines heal and to get adequate protein
while being sick or immediately after having c diff
there is NO EVIDENCE to support this idea. In addition,
many people find themselves
being lactose intolerant after having c diff and many protein
drinks contain lactose. (Lactose is a sugar contained in most
dairy products: milk, yogurt, cheese, etc.)
REFERENCE:
Protein Supplements to do NOT Help heal the intestines
3. Don't Eat a High-Fat Diet
A study compared a high-fat (low-fiber) diet to a
low-fat (low-fiber) diet on mice who had been infected with c diff.
1. High-fat (low-fiber) was called the Western Diet
2. Low-fat (low-fiber) = LF/LF Diet
The mice fed the Western Diet had a significantly higher death rate than
the LF/LF Diet.
CAUTION: The study only examined a high fat-diet accompanied
with a low-fiber
diet; therefore, it is not known for certain if it was the high fat part of
the diet alone that caused the increase in mortality. It could have
been from the combination of high fat and low fiber, NOT just because of
the fat in the diet.
A second study examined how a high-fat/high-protein diet (like the Atkins
Diet) increased the chance of c diff mortality by decreasing protective
bacteria (Lachnospiraceae and Ruminococcaceae).
This study compared three different diets:
1. high-fat/high-protein diet
2. high-fat/low-protein diet
3. carbohydrate/low-fiber diet.
Both of the high-fat diets
increased the chance of c diff mortality. The high-fat/high-protein diet
did it consitently; where as, the high-fat/low-protein diet had
mixed results.
The carbohydrate/low-fiber diet had the least
amount of illness.
REFERENCE: A High-Fat/High-Protein
Diet Increase C diff
A general population study empphasized the
potential harm of excessive fat intake.
However, this study was NOT specific to c diff.
It found that there was approximately a 5% increase in
deaths due to the consumption of excess dietary fat.
This was a meta analysis of 19 different studies. This meta analysis
contained over a million people in it and was conducted over
many years.
It demonstrated an association of a high-fat diet with
several illness, primarily cardiovascular disease and
cancers.
Caution: The total suggested dietary-fat for a day should be
about 20-35% of a person's total calorie count.
A minumum suggested amount of fat each
day is 20% of total daily calories.
Too little dietary fat, just like too much dietary fat
can also be detrimental.
High-Fat/Low-Fiber Increase Morality REFERENCE

4. Don't Eat A High-Calcium Diet
There is a study that found that feeding mice a calcium-deprived diet
reduced the c diff relapse in mice by 90%. The study found that calcium
is a necessary mineral needed for c diff to germinate (in mice).
CAUTION: It is important to remember the humans need a certain
amount of calcium in there diet, primarily to have strong bones;
however, they rarely need calcium supplements, and they are able
to go without
calcium foods for a period of time without reprocussions.
This study infers that if a person is at a
high risk for a c diff infection, that person MIGHT try
decreasing their calcium intake for a short period of time
to prevent relapsing.
However, it should always be remembered that this study was on mice,
and mice are vastly different from humans.
Not all results from mice studies hold true to people.
REFERENCE: Calcium-Deprived Diet
5. Don't Eat a High-Sugar Diet
A mice study found that
mice fed a VERY high-sucrose diet significantly increased their
mortality rate. The mice were fed a diet that contained 94% sucrose
(table sugar),
and the rest was from cornstarch and maltodextrin.
Caution: The
above study fed mice a diet that was 94% sucrose (table sugar).
The typical American diet has approximately 10-13% simple sugar.
The world
Health Association states that up 10% of a person's
daily calorie intake can be in the form of simple sugars, such
as table sugar. However, there is NO MINIMUM requirement
for the intake of simple sugars. A person can easily live
without the intake of simple sugar.
REFERENCE: A High-Sugar Diet is Bad
6. Don't Eat Excessive Salt

One study that found that
high-salt diets will decrease Lactobacillus Bacteria
(which is considered a good bacterium). Salt has also been
reported to cause c diff to
adhere to the colon wall better. Therefore, there is circumstantial
evidence that a high-salt diet MIGHT be detrimental to
a person trying to prevent c diff.
REFERENCE 1: Salt Decreases Good Gut Bacteria
REFERENCE 2: C diff Is Able to Adapt to High-Salt Environment
7. Don't Drink Excessive Alcohol
 One study on alchol abuse and c diff found
that if people abuse alcohol there is about a 2 fold risk of c diff
infection. However, the study subjects were
ALL known to be alcoholics, not just occasional alcohol drinkers.
Thus, there is some evidence
that drinking alcohol excessively will increase the risk
of c diff infection and
relapse, but there is no evidence that the same is true
for light-alcohol users.
One study on alchol abuse and c diff found
that if people abuse alcohol there is about a 2 fold risk of c diff
infection. However, the study subjects were
ALL known to be alcoholics, not just occasional alcohol drinkers.
Thus, there is some evidence
that drinking alcohol excessively will increase the risk
of c diff infection and
relapse, but there is no evidence that the same is true
for light-alcohol users.
However, there is also evidence that alcohol abuse is associated with
higher rates of inflammatory Bowel Disease (IBD). But,
once again, the studies indicate that there is a higher rate of
IBD among alcohol abuses, but don't define how much risk is
generated by drinking small amounts of alcohol.
REFERENCE:
Alcohol Increases Risk of C Diff
REFERENCE:
Alcohol Increases Risk of IBD
DOs
1. DO Consider a Low FODMAP Diet
During an infection with c diff, or immediately after
a c diff infection, many people will develop
post-infection irritable bowel syndrome (PI-IBS).
During this period of time
a person MIGHT need to follow a "Low" FODMAP diet
for a period of time. This period of time
is NOT clearly defined. It seems to vary between
a few weeks to many years. Ideally a low FODMAP diet
should NOT be followed for more than a couple of
months because eating a low FODMAP diet
can cause a decrease in a person's
good gut bacteria, which can inturn increase their
chance of c diff relapse.
FODMAP is an ancronym for for Fermentable Oligosaccharides,
Disaccharides, Monosaccharides, And Polyols.
These are short-chain carbohydrates that are
poorly absorbed in the small intestine and can
cause digestive issues
like gas, bloating, and diarrhea.
HOWEVER, these SAME
short-chain carbohydrates can increase the number
of good bacteria in the gut, and thereby decrease the
chance of c diff infection or relapse. Therefore,
while a LOW FODMAP diet MIGHT be necessary for some
period time after a person has c diff, it should not
be continued longer than it is necessary.
Low FODMAP foods are foods such as:
eggplant, green beans, bok choy, carrot, cucumber,
potato, oats, gluten free pasta, white rice, rice cakes,
sourdough bread, white bread, dark chocolate,
maple syrup, table sugar, eggs, firm tofu,
plain cooked meats, poultry and seafood.
REFERENCE: Low-FODMAP Diet for IBS
Caution: It is important to remember that some of the
food mentioned in a low-FODMAP diet are HIGH in protein
and some studies have indicated that a low protein/low fat
diet can reduce the chance of c diff relapse.
2. DO Consider an Elimination Diet
 If a person has Post Infection-Irritable Bowel Syndrome
and cannot tolerate the foods on the Low-FODMAP diet
they may want to consider an an "Elimination Diet."
An elimination diet is similar to the aforementioned Low-
FODMAP Diet, BUT is even more limited in the foods that
can be eaten. It also should not be continued any longer
than is absolutely necessary, because by eliminating
numerous foods a person can reduce the number of good
gut bacteria, which can be helpful to reduce the
chance of c diff infection.
If a person has Post Infection-Irritable Bowel Syndrome
and cannot tolerate the foods on the Low-FODMAP diet
they may want to consider an an "Elimination Diet."
An elimination diet is similar to the aforementioned Low-
FODMAP Diet, BUT is even more limited in the foods that
can be eaten. It also should not be continued any longer
than is absolutely necessary, because by eliminating
numerous foods a person can reduce the number of good
gut bacteria, which can be helpful to reduce the
chance of c diff infection.
There are two basic methods by which an elimination diet can
be done.
The first method is for a person to remove ALL the foods
from their diet that they
think are bothering them. After they are better
for a period time, they can test one additional new food
at a time to determine if they are able to tolerate the new food.
By increasing the diversity of their diet, they should
be able to increase the diveristy of the good bacteria in
their colon.
A second method of doing an elimination diet
is where ALL foods except either rice and
water or bread and water are removed.
After a period of time when their
gut feels reasonably well they start
testing one food at a time, watching each food for a reaction.
If a food can NOT be tolerated, then it should be temporarily eliminated.
Once a person feels better again, they can try a new food.
Each new food is usually tested for a couple of days before
testing another food. Foods that seem to cause a problem
can be retried when a person is
feeling better to determine if they are still intolerable.
REFERENCE: Elimination Diet for C Diff
3. DO Consider Eating Some Fermented Foods

The word "condsider" is used because some people
cannot tolerate fermented foods. In addition,
some fermented foods such as Yogurt and Kefir
contain high amount of calcium, which a person MIGHT
be trying to avoid after having c diff.
There was one small study, using 36 HEALTHY people, that studied how
fermented foods, "OR" a high-fiber diet influenced
the gut microbiome.
In this study, 36 subjects at Stanford were
grouped into one of two groups, one group ate a high-fiber diet,
and one group that ate a diet high in fermented
foods. All subjects were followed for 10 weeks.
The study found that
eating fermented foods three times a day
increased gut bacteria diversity, which in turn
reduced gut inflammatory markers. In contrast, the study also
found that eating a high-fiber diet for 10 weeks
did not change the gut bacteria.
REFERENCE: Fermented Food Reduces Gut Inflammation
Examples of Fermented Foods:
Kombucha (No Sugar Added)
Fermented Vegetables
Tempeh (Gluten-Free)
Miso (Refrigerated)
Pickles (In salt, Not vinegar)
Sauerkraut (Refrigerated)
Kimchi
Kefir
Plain Yogurt (Those marked Live Culture are probably better.)
Cottage Cheese (Those marked Live Culture are probably better.)
Certain aged cheeses (Check label for live and active cultures)
CAUTION: People with C diff were NOT used
for this study; therefore, the studies results MIGHT NOT
be APPLICABLE to people who have their intestines
inflamed or depleted of good intestinal bacteria due to a recent
c diff infection.
In addition, an increased diveristy of gut microbiomes does NOT
guarantee a person will have less c diff.
Lastly, one study found that eating yogurt increased
streptococcus bacteria--
but, at the same time decreased odoribacter bacteria.
The odoribacter bacteria is also considered to be
a good gut bacteria.
Thus, the overall benefit of eating yogurt
might not be as good as hoped.
REFERENCE: Eating Yogurt Decreases Odoribacter Bacteria
4. DO Consider Eating High-FODMAP Foods

The word "consider" is used because after a person has
had c diff, there intestines are oftentimes more sensitive
to all different types of foods, especially FODMAP foods.
However, FODMAPS foods are high in soluble fiber
and a diet high in soluble fiber has been found
to be protective against c diff.
If a person does not have PI-IBS and wants
to try to diversify their gut bacteria,
they can try to eat to some of the following FODMAP foods.
Oatmeal Cereal, peas, beans, apples,
bananas, avocados, citrus fruits, carrots, barley and psyllium.
Fiber Chart
A mice study found that mice that were fed a high-
soluble-fiber diet
produced MORE ACETATE in their intestine.
This increase in acetate helped regulate the immune response in
the protective layer of the colon. This in turn
was found to help protect against c diff.
REFERENCE: A High-Soluble-Fiber Diet Improves the
Immune System in Mice
CAUTION: A small study on humans found that
humans who ate a high-fiber diet for 10 weeks were unable to
change their intestinal bacteria.
5. DO Consider Eating Some Fruit (Apples, Oranges, Lemons, Berries)
Apples, oranges, lemons, and berries contain pectin and this pectin
has been found to be beneficial.
A study on mice found that the pectin helped
to improve intestinal integrity and
increase Lachnospiraceae bacteria in the intestine. Higher levels of
Lachnospiraceae bacteria are associated with better health.
MACs Reduce C diff in Mice Reference
Reference: Pectin
Might Decrease C diff in Mice
CAUTION: Fruits are FODMAP foods; therefore, if
a person has IBS or PI-IBS these foods may be hard to tolerate.
6. Do Drink Sufficient Water
Some people may decrease their fluid intake
to try minimize their diarrhea.
However, when a person is having loose bowel movements
or diarrhea they have
an increased chance to become dehydrated.
When a person is dehydrated they will often
not feel well; however, beyond not feeling well
being dehydrated can in some cases lead to kidney
damage and in extreme cases dehydration can cause death.
The average amount of fluids a person should drink in
a day is 1500 ml. 1500 ml is equal to 50 ounces of fluid,
or approximately three 500 ml bottles or water, or six
8 ounce glasses of water. However, if a person has diarrhea,
there if often a need for even more fluid.
In the worst case of dehydration, a person may need to get
fluids intravenously.
Caution: While being correctly hydrated is very important
to good health, excess fluids can be a problem as well.
Although, overhydration does not occur that often it can
cause excessive urination and a lowered sodium in the blood.
The lowered sodium is called hyponatremia, and it will also
cause a person feel poorly.
In addition, a person MUST be cautious when hydrating themselves.
Some electrolyte solutions such as Gatorade and Powerade
can actually cause diarrhea. It is best to try to hydrate
with a solution that contains a little salt and sugar. A person
can make their own or by Pedialyte.
SPECIFIC FOODS
1. Kefir

There is one study that reported that Kefir will favorably
change the gut microbiome.
Kefir was found to primarily increase Acetinobacteria.
Acetinobacteria is thought to
be a bacterium that is beneficial to the gut. It is hoped that
an increase in acetinobateria will
inhibit the growth of c diff spores.
CAUTION: The study that was done
only proved that kefir increase acetinobacteria,
it did not prove this increase
in acetinobacteria would decrease the rate of c diff infection or relapse.
Reference: Kefir
2. Yogurt

Yogurt probably has some short-term benefits on the
gut microbiomes.
A study has reported that a short-term increase in
Streptococcus Thermophilus and Bifidobacterium Animalis bacteria
among people eating yogurt.
These two bacteria are considered to be good gut bacteria.
However, another study found that was while they found an increase
in Streptococcus bacteria among regular yogurt eaters, it also found
a decrease in odoribacter bacteria. This odoribacter bacteria
is also considered a beneficial
gut bacterium. Thus, there is a chance that too much yogurt
MIGHT be detrimental.
REFERENCE 1: Yogurt Support
REFERENCE 2: Yogurt Support
REFERENCE 3: Yogurt Decreases Odoribacter Bacterium
CAUTION: Not all yogurts are made the same; therefore, some yogurt brands
MIGHT be more beneficial than others.
Most yogurt studies do NOT include the brand of the yogurt used,
and they don't compare one yogurt brand to another.
They also don't identify the starter bacteria (Lactobacillus
Bulgaricus, Streptococcus Thermophilus,
Bifidobacterium Lactis or Lactobacillus Acidophilus) that were used
to start the yogurt; therefore, the specific probiotics that are
produced by the yogurt is not known.
Starter bacteria are the bacteria that are used to cause
fermentation of the yogurt, and they can vary.
Starter bacteria include the following:
Lactobacillus Bulgaricus, Streptococcus Thermophilus,
Bifidobacterium Lactis or Lactobacillus Acidophilus.
The starter bacteria determine
the probiotics
that are produced at the end of the fermentation process.
Generally, yogurts labeled "Live Active Culture" are
considered to have more probiotics. A couple of the brands
that meet this criteria are the following:
Chobani, Activia, Stonyfield, FAGE, and Siggi's.
But, there are no studies
that prove one yogurt brand is better than the other.
3. Plantains

There was a study on one specific food, called plantains
and c diff. In the study, plantains were
found to both inhibit c diff and decrease
the ability of c diff bacteria to stick to the wall of the intestines.
CAUTION: This study was ONLY DONE in the laboratory;
thus, the effect on eating plantains by humans
is unknown.
Reference: Plantain Are Beneficial
Reference: Plantain Supplement
DIET SUMMARY
A diet for C diff is COMPLICATED.
It needs to be INDIVIDUALIZED and adjusted over time.
In addition, there are no tests available to determine if
a person is eating the right foods to attain the ideal
gut microbiome.
There are NO foods or diets that are definitely helpful
because there are no studies that have determined
what the ideal gut microbiomes are, and there are no
tests that an individual can do to determine if they are
moving toward the perfect gut microbiome. (There is a
GI Panel Test available, which tests about 40 gut bacteria,
but there are over 500 gut bacteria, and the GI Panel test
only test for about 40.)
Because of these difference, there are a variety of
diet suggestions.
EACH PERSON MUST CONSIDER THEIR OWN CIRCUMSTANCES
BEFORE MAKING ADJUSTMENT TO THEIR DIET.
Lastly, it must be mentioned that a person might NOT NEED
to alter their diet at all.
1. A person could choose to simply take the antibiotics for
c diff and eat a regular diet.
This works for some people.
2. A person could choose to take medications that are used
for Irritable Bowel Syndrome and eat a regular diet.
Medications for IBS are medications such as Bentyl, Imodium,
Elavil, and Nortriptyline. These work for some people--but
they OFTEN have side effects.
3. A person could try a variety of supplements and
continue to eat their regular diet.
These supplements include, but are not limited to
Florastor, Bentonite Clay, and Black Seed Oil.
These treatments also sometimes work.
They are explained in another section
of this website.
CAUTION ON ALL DIET INFORMATION
Before anyone adjusts their diets,
they should be aware that there
are four problems with the studies that have been done.
The first problem is that rodents and humans
have vastly different intestines.
Not only is the shape of rodents’ intestines different,
but rodents have different normal gut bacteria.
The second problem is that the only study that was done on people
was done on HEALTHY people NOT people who are
infected with c diff. A person who is infected
with c diff and has an inflamed or irritated colon
MIGHT NOT respond the same way as a healthy person does.
The third problem is that laboratory studies (in vitro) have no
test on living organism; therefore, their applicability to people
infected with c diff is even more distant than the relationship
between mice and humans.
The fourth problem is that there are
conflicting reports between different studies.
These problems within these studies does NOT mean they should
be totally disregarded, but it does mean that they can
NOT be TOTALLY RELIED UPON.
VI. What ARE NEW TREATMENTS BEING STUDIED?
*If you want to see if there are any new treatment studies
that are going on in the United States you can check the following
website, https://clinicaltrials.gov.
Click Here
1. VE303 (RESTORATiVE303)
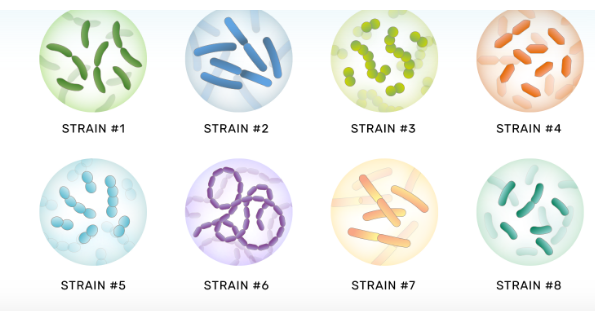 VE303 is one of the more promising new treatments for c diff.
It is a new type of FMT that is being tested and thus
far has been found to be about as effective as Vowst.
However, this type of FMT is different from Vowst because
VE303 it is NOT made from human excrement. Vowst is.
Instead, VE303 is
made from 8 specific bacteria, which are grown in a
laboratory. The advantage of VE303 over Vowst is that
there is less risk of adverse effects. This treatment is
currently in Phase 3 and is looking for participants.
VE303 is one of the more promising new treatments for c diff.
It is a new type of FMT that is being tested and thus
far has been found to be about as effective as Vowst.
However, this type of FMT is different from Vowst because
VE303 it is NOT made from human excrement. Vowst is.
Instead, VE303 is
made from 8 specific bacteria, which are grown in a
laboratory. The advantage of VE303 over Vowst is that
there is less risk of adverse effects. This treatment is
currently in Phase 3 and is looking for participants.
Phase 3 Study Looking for Particpants
2. DAV132

DAV132 is an enteric-coated activated charcoal.
Enteric coated means it has a hard outer shell designed to
prevent the pill from being broken down in the small intestines, but rather
being broken down in the large intestines. Once it is broken down in the
large intestines the activated charcoal will absorb unwanted antibiotics
while
preserving the good intestinal bacteria.
Two research studies have demonstrated
that it is partially effective, but further
research still needs to be done.
It is currently in phase 2 trials; But, the trials are being
conducted in France, Bulgaria, Serbia and France. There are none
in the United States.
3. Ebselen
Ebselen is a medication is currently being studied
for the treatment for Meniere's disease; however,
some researchers have also looked at it for the use
in treating c diff.
One study on mice showed that ebselen decreased
intestinal inflammation and damage due to c diff toxins.
The problem with this information, is the study was done on mice and
there are no studies currently being done on ebselen for the
purpose of treating c diff. There are studies researching
the effectiveness on Meniere's disease, cochlear implants,
and depression--but none regarding c diff.
Thus, the effectiveness on people who have c diff
has yet to be proven. Perhaps more information will be
gained on the effectiveness of ebselen for c diff through the other
investigational studies.
Reference 1: Ebselen for C diff
Reference 2: Ebselen for C diff
Reference 3: Ebselen for C diff
4. SYN-004 (Ribaximase)
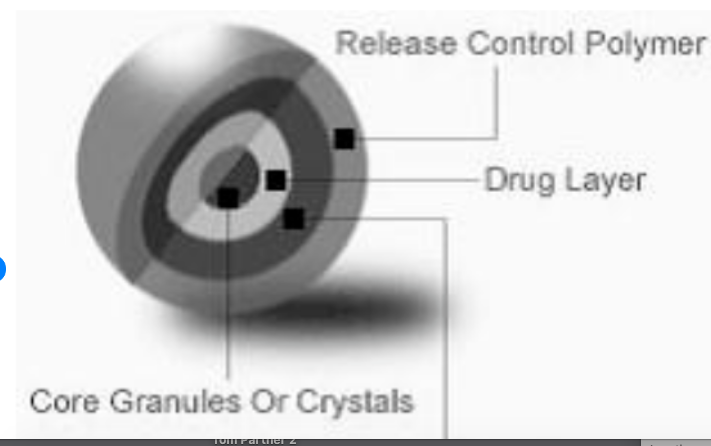
SYN004 (ribaximase) is a medication designed to break down
beta-lactam antibiotics after they have entered the large intestines.
Beta-lactam antibiotics are
antibiotics such as penicillin, amoxicillin, Keflex and Rocephin.
One study reported that
ribaximase did reduce the percentage of people who got c diff while
taking it; however, the same study showed that those people
who received rebaximase had substantially more adverse effects. The
authors reported that they thought the adverse effects where
coincidental.
There is currently a study being conducted that may
determine the effectiveness and chance of adverse effects; but
the trial is in Missouri, and it is only on people who are receiving treatment
for a severe blood disease.
Reference: SYN004
Reference: American College of Gastroenterology
2. Antidiarrheal agents:
 A. Bismuth Subsalicylate (BSS) (Pepto Bismol) - has antibacterial properties against C. Diff. ;
therefore,
might be of some benefit in treating C. Diff.
A. Bismuth Subsalicylate (BSS) (Pepto Bismol) - has antibacterial properties against C. Diff. ;
therefore,
might be of some benefit in treating C. Diff.
Reference: Pepto Bismol
B. INITIALLY, Imodium and Lomotil are not recommended to treat C. Diff. because they have no anti C. Diff. qualities and may indirectly increase the toxins that affect the large intestine. However, they can sometimes be used after c diff antibiotics are started. However, they must be used judiciously to avoid causing constipation or interfering with the desired actions of the c. diff antibiotics.
 3. Fecal Microbial Transplant (FMT):
3. Fecal Microbial Transplant (FMT):A. FMT via a colonoscopy (~91% cure rate)
B. FMT via a nasal gastric tube (~81% cure rate
C. FMT via pills (Vowst) FDA approved in 2024 (~96% cure rate)
D. FMT via enema (Rebyota) (~83% cure rate)

DON'TS
1. Don't Eat a High-Protein Diet
2. Don't Eat a High-Fat Diet
3. Don't Drink Protein Drinks or Shakes
4. Don't Eat a High-Calcium Diet
5. Don't Eat a High-Sugar Diet
6. Don't Eat a Lot of Salt
7. Don't Drink a lot of Alcohol
DOs
Some foods of food groups that you should probably eat or drink.
1. Do Consider a Low FODMAP Diet
2. Do Consider an Elimination Diet
3. Do Consider Eating Some Formented Foods
4. Do Consider Eating Some High-FODMAP Foods
3. Do Consider Eating Some Fruits
6. Do Drink SUFFICIENT Water
1. Don't Eat a Lot of Protein
There was a study of two groups of mice fed a relatively similar
diets but the diets differed in the amount of protein and
fat. Diet 5010 contained approximately 24% protein and 10% fat
and, and Diet 5053 contained approximately 20% protein and 5% fat.
Both groups of mice were infected with c diff, but the group
that were fed Diet 5053 (20% protein and 5% fat diet) had less colon
inflammation (colitis).
REFERENCE:
Lower
Protein and Fat Diet decreases C diff Severity
A second reason that protein consumption is probably not a good idea
is that a second mice study found that reducing glycine among hamsters
reduced their rate of dying. (Glycine is a type of protein that is found
in most types of animals (meat, foul, and fish) and to a lesser extent
in many types of beans.
This study is more complicated than simply not feeding hamsters
glycine, instead the researchres
created a type of c diff bacteria that was unable
to digest glycine. The researchers just infected hamsters with
their created bacteria versus a group of hamsters infected with the
average c diff bacteria. The hamsters given the created c diff
lived longer before dying than the other hamsters.
REFERENCE:
Glycine Reducation Diet Reduces C Diff among Infected Hamsters
A third study also found a correlation between a high-animal protein
diet (meat) and decreased levels of
Eubacterium Rectale and Roseburia Intinalis Bacteria.
Both of these bacteria
produce butyrate, and butyrate reduces inflammation. Therefore,
these bacteria are considered good gut bacteria.
REFERENCE:
High-Animal-Protein Diet is Correlated with Inflammatory Bowed Disease Reference
In reality, it is nearly impossible to avoid all protein and it
would not be healthy for a person to avoid
all protein for a long period of time;
however, it is possible to decrease the amount of protein
eaten for a short period of time
in the hopes that it might
decrease the chance of c diff relapse.
REFERENCE: High Red Meat Consumption is Correlated with Cancer,
Heart Disase, and Kidney Disease Referenc
2. Don't Drink Protein Supplements
A study tested 17 different
sources of protein in protein drinks and found that NONE of them
were beneficial to the colon.
Although protein supplements might sound like a logical way to help
the intestines heal and to get adequate protein
while being sick or immediately after having c diff
there is NO EVIDENCE to support this idea. In addition,
many people find themselves
being lactose intolerant after having c diff and many protein
drinks contain lactose. (Lactose is a sugar contained in most
dairy products: milk, yogurt, cheese, etc.)
REFERENCE:
Protein Supplements to do NOT Help heal the intestines
3. Don't Eat a High-Fat Diet
A study compared a high-fat (low-fiber) diet to a
low-fat (low-fiber) diet on mice who had been infected with c diff.
1. High-fat (low-fiber) was called the Western Diet
2. Low-fat (low-fiber) = LF/LF Diet
The mice fed the Western Diet had a significantly higher death rate than
the LF/LF Diet.
CAUTION: The study only examined a high fat-diet accompanied
with a low-fiber
diet; therefore, it is not known for certain if it was the high fat part of
the diet alone that caused the increase in mortality. It could have
been from the combination of high fat and low fiber, NOT just because of
the fat in the diet.
A second study examined how a high-fat/high-protein diet (like the Atkins
Diet) increased the chance of c diff mortality by decreasing protective
bacteria (Lachnospiraceae and Ruminococcaceae).
This study compared three different diets:
1. high-fat/high-protein diet
2. high-fat/low-protein diet
3. carbohydrate/low-fiber diet.
Both of the high-fat diets
increased the chance of c diff mortality. The high-fat/high-protein diet
did it consitently; where as, the high-fat/low-protein diet had
mixed results.
The carbohydrate/low-fiber diet had the least
amount of illness.
REFERENCE: A High-Fat/High-Protein
Diet Increase C diff
A general population study empphasized the
potential harm of excessive fat intake.
However, this study was NOT specific to c diff.
It found that there was approximately a 5% increase in
deaths due to the consumption of excess dietary fat.
This was a meta analysis of 19 different studies. This meta analysis
contained over a million people in it and was conducted over
many years.
It demonstrated an association of a high-fat diet with
several illness, primarily cardiovascular disease and
cancers.
Caution: The total suggested dietary-fat for a day should be
about 20-35% of a person's total calorie count.
A minumum suggested amount of fat each
day is 20% of total daily calories.
Too little dietary fat, just like too much dietary fat
can also be detrimental.
High-Fat/Low-Fiber Increase Morality REFERENCE

4. Don't Eat A High-Calcium Diet
There is a study that found that feeding mice a calcium-deprived diet
reduced the c diff relapse in mice by 90%. The study found that calcium
is a necessary mineral needed for c diff to germinate (in mice).
CAUTION: It is important to remember the humans need a certain
amount of calcium in there diet, primarily to have strong bones;
however, they rarely need calcium supplements, and they are able
to go without
calcium foods for a period of time without reprocussions.
This study infers that if a person is at a
high risk for a c diff infection, that person MIGHT try
decreasing their calcium intake for a short period of time
to prevent relapsing.
However, it should always be remembered that this study was on mice,
and mice are vastly different from humans.
Not all results from mice studies hold true to people.
REFERENCE: Calcium-Deprived Diet
5. Don't Eat a High-Sugar Diet
A mice study found that
mice fed a VERY high-sucrose diet significantly increased their
mortality rate. The mice were fed a diet that contained 94% sucrose
(table sugar),
and the rest was from cornstarch and maltodextrin.
Caution: The
above study fed mice a diet that was 94% sucrose (table sugar).
The typical American diet has approximately 10-13% simple sugar.
The world
Health Association states that up 10% of a person's
daily calorie intake can be in the form of simple sugars, such
as table sugar. However, there is NO MINIMUM requirement
for the intake of simple sugars. A person can easily live
without the intake of simple sugar.
REFERENCE: A High-Sugar Diet is Bad
6. Don't Eat Excessive Salt

One study that found that
high-salt diets will decrease Lactobacillus Bacteria
(which is considered a good bacterium). Salt has also been
reported to cause c diff to
adhere to the colon wall better. Therefore, there is circumstantial
evidence that a high-salt diet MIGHT be detrimental to
a person trying to prevent c diff.
REFERENCE 1: Salt Decreases Good Gut Bacteria
REFERENCE 2: C diff Is Able to Adapt to High-Salt Environment
7. Don't Drink Excessive Alcohol
 One study on alchol abuse and c diff found
that if people abuse alcohol there is about a 2 fold risk of c diff
infection. However, the study subjects were
ALL known to be alcoholics, not just occasional alcohol drinkers.
Thus, there is some evidence
that drinking alcohol excessively will increase the risk
of c diff infection and
relapse, but there is no evidence that the same is true
for light-alcohol users.
One study on alchol abuse and c diff found
that if people abuse alcohol there is about a 2 fold risk of c diff
infection. However, the study subjects were
ALL known to be alcoholics, not just occasional alcohol drinkers.
Thus, there is some evidence
that drinking alcohol excessively will increase the risk
of c diff infection and
relapse, but there is no evidence that the same is true
for light-alcohol users.
However, there is also evidence that alcohol abuse is associated with
higher rates of inflammatory Bowel Disease (IBD). But,
once again, the studies indicate that there is a higher rate of
IBD among alcohol abuses, but don't define how much risk is
generated by drinking small amounts of alcohol.
REFERENCE:
Alcohol Increases Risk of C Diff
REFERENCE:
Alcohol Increases Risk of IBD
DOs
1. DO Consider a Low FODMAP Diet
During an infection with c diff, or immediately after
a c diff infection, many people will develop
post-infection irritable bowel syndrome (PI-IBS).
During this period of time
a person MIGHT need to follow a "Low" FODMAP diet
for a period of time. This period of time
is NOT clearly defined. It seems to vary between
a few weeks to many years. Ideally a low FODMAP diet
should NOT be followed for more than a couple of
months because eating a low FODMAP diet
can cause a decrease in a person's
good gut bacteria, which can inturn increase their
chance of c diff relapse.
FODMAP is an ancronym for for Fermentable Oligosaccharides,
Disaccharides, Monosaccharides, And Polyols.
These are short-chain carbohydrates that are
poorly absorbed in the small intestine and can
cause digestive issues
like gas, bloating, and diarrhea.
HOWEVER, these SAME
short-chain carbohydrates can increase the number
of good bacteria in the gut, and thereby decrease the
chance of c diff infection or relapse. Therefore,
while a LOW FODMAP diet MIGHT be necessary for some
period time after a person has c diff, it should not
be continued longer than it is necessary.
Low FODMAP foods are foods such as:
eggplant, green beans, bok choy, carrot, cucumber,
potato, oats, gluten free pasta, white rice, rice cakes,
sourdough bread, white bread, dark chocolate,
maple syrup, table sugar, eggs, firm tofu,
plain cooked meats, poultry and seafood.
REFERENCE: Low-FODMAP Diet for IBS
Caution: It is important to remember that some of the
food mentioned in a low-FODMAP diet are HIGH in protein
and some studies have indicated that a low protein/low fat
diet can reduce the chance of c diff relapse.
2. DO Consider an Elimination Diet
 If a person has Post Infection-Irritable Bowel Syndrome
and cannot tolerate the foods on the Low-FODMAP diet
they may want to consider an an "Elimination Diet."
An elimination diet is similar to the aforementioned Low-
FODMAP Diet, BUT is even more limited in the foods that
can be eaten. It also should not be continued any longer
than is absolutely necessary, because by eliminating
numerous foods a person can reduce the number of good
gut bacteria, which can be helpful to reduce the
chance of c diff infection.
If a person has Post Infection-Irritable Bowel Syndrome
and cannot tolerate the foods on the Low-FODMAP diet
they may want to consider an an "Elimination Diet."
An elimination diet is similar to the aforementioned Low-
FODMAP Diet, BUT is even more limited in the foods that
can be eaten. It also should not be continued any longer
than is absolutely necessary, because by eliminating
numerous foods a person can reduce the number of good
gut bacteria, which can be helpful to reduce the
chance of c diff infection.
There are two basic methods by which an elimination diet can
be done.
The first method is for a person to remove ALL the foods
from their diet that they
think are bothering them. After they are better
for a period time, they can test one additional new food
at a time to determine if they are able to tolerate the new food.
By increasing the diversity of their diet, they should
be able to increase the diveristy of the good bacteria in
their colon.
A second method of doing an elimination diet
is where ALL foods except either rice and
water or bread and water are removed.
After a period of time when their
gut feels reasonably well they start
testing one food at a time, watching each food for a reaction.
If a food can NOT be tolerated, then it should be temporarily eliminated.
Once a person feels better again, they can try a new food.
Each new food is usually tested for a couple of days before
testing another food. Foods that seem to cause a problem
can be retried when a person is
feeling better to determine if they are still intolerable.
REFERENCE: Elimination Diet for C Diff
3. DO Consider Eating Some Fermented Foods

The word "condsider" is used because some people
cannot tolerate fermented foods. In addition,
some fermented foods such as Yogurt and Kefir
contain high amount of calcium, which a person MIGHT
be trying to avoid after having c diff.
There was one small study, using 36 HEALTHY people, that studied how
fermented foods, "OR" a high-fiber diet influenced
the gut microbiome.
In this study, 36 subjects at Stanford were
grouped into one of two groups, one group ate a high-fiber diet,
and one group that ate a diet high in fermented
foods. All subjects were followed for 10 weeks.
The study found that
eating fermented foods three times a day
increased gut bacteria diversity, which in turn
reduced gut inflammatory markers. In contrast, the study also
found that eating a high-fiber diet for 10 weeks
did not change the gut bacteria.
REFERENCE: Fermented Food Reduces Gut Inflammation
Examples of Fermented Foods:
Kombucha (No Sugar Added)
Fermented Vegetables
Tempeh (Gluten-Free)
Miso (Refrigerated)
Pickles (In salt, Not vinegar)
Sauerkraut (Refrigerated)
Kimchi
Kefir
Plain Yogurt (Those marked Live Culture are probably better.)
Cottage Cheese (Those marked Live Culture are probably better.)
Certain aged cheeses (Check label for live and active cultures)
CAUTION: People with C diff were NOT used
for this study; therefore, the studies results MIGHT NOT
be APPLICABLE to people who have their intestines
inflamed or depleted of good intestinal bacteria due to a recent
c diff infection.
In addition, an increased diveristy of gut microbiomes does NOT
guarantee a person will have less c diff.
Lastly, one study found that eating yogurt increased
streptococcus bacteria--
but, at the same time decreased odoribacter bacteria.
The odoribacter bacteria is also considered to be
a good gut bacteria.
Thus, the overall benefit of eating yogurt
might not be as good as hoped.
REFERENCE: Eating Yogurt Decreases Odoribacter Bacteria
4. DO Consider Eating High-FODMAP Foods

The word "consider" is used because after a person has
had c diff, there intestines are oftentimes more sensitive
to all different types of foods, especially FODMAP foods.
However, FODMAPS foods are high in soluble fiber
and a diet high in soluble fiber has been found
to be protective against c diff.
If a person does not have PI-IBS and wants
to try to diversify their gut bacteria,
they can try to eat to some of the following FODMAP foods.
Oatmeal Cereal, peas, beans, apples,
bananas, avocados, citrus fruits, carrots, barley and psyllium.
Fiber Chart
A mice study found that mice that were fed a high-
soluble-fiber diet
produced MORE ACETATE in their intestine.
This increase in acetate helped regulate the immune response in
the protective layer of the colon. This in turn
was found to help protect against c diff.
REFERENCE: A High-Soluble-Fiber Diet Improves the
Immune System in Mice
CAUTION: A small study on humans found that
humans who ate a high-fiber diet for 10 weeks were unable to
change their intestinal bacteria.
5. DO Consider Eating Some Fruit (Apples, Oranges, Lemons, Berries)
Apples, oranges, lemons, and berries contain pectin and this pectin
has been found to be beneficial.
A study on mice found that the pectin helped
to improve intestinal integrity and
increase Lachnospiraceae bacteria in the intestine. Higher levels of
Lachnospiraceae bacteria are associated with better health.
MACs Reduce C diff in Mice Reference
Reference: Pectin
Might Decrease C diff in Mice
CAUTION: Fruits are FODMAP foods; therefore, if
a person has IBS or PI-IBS these foods may be hard to tolerate.
6. Do Drink Sufficient Water
Some people may decrease their fluid intake
to try minimize their diarrhea.
However, when a person is having loose bowel movements
or diarrhea they have
an increased chance to become dehydrated.
When a person is dehydrated they will often
not feel well; however, beyond not feeling well
being dehydrated can in some cases lead to kidney
damage and in extreme cases dehydration can cause death.
The average amount of fluids a person should drink in
a day is 1500 ml. 1500 ml is equal to 50 ounces of fluid,
or approximately three 500 ml bottles or water, or six
8 ounce glasses of water. However, if a person has diarrhea,
there if often a need for even more fluid.
In the worst case of dehydration, a person may need to get
fluids intravenously.
Caution: While being correctly hydrated is very important
to good health, excess fluids can be a problem as well.
Although, overhydration does not occur that often it can
cause excessive urination and a lowered sodium in the blood.
The lowered sodium is called hyponatremia, and it will also
cause a person feel poorly.
In addition, a person MUST be cautious when hydrating themselves.
Some electrolyte solutions such as Gatorade and Powerade
can actually cause diarrhea. It is best to try to hydrate
with a solution that contains a little salt and sugar. A person
can make their own or by Pedialyte.
SPECIFIC FOODS
1. Kefir

There is one study that reported that Kefir will favorably
change the gut microbiome.
Kefir was found to primarily increase Acetinobacteria.
Acetinobacteria is thought to
be a bacterium that is beneficial to the gut. It is hoped that
an increase in acetinobateria will
inhibit the growth of c diff spores.
CAUTION: The study that was done
only proved that kefir increase acetinobacteria,
it did not prove this increase
in acetinobacteria would decrease the rate of c diff infection or relapse.
Reference: Kefir
2. Yogurt

Yogurt probably has some short-term benefits on the
gut microbiomes.
A study has reported that a short-term increase in
Streptococcus Thermophilus and Bifidobacterium Animalis bacteria
among people eating yogurt.
These two bacteria are considered to be good gut bacteria.
However, another study found that was while they found an increase
in Streptococcus bacteria among regular yogurt eaters, it also found
a decrease in odoribacter bacteria. This odoribacter bacteria
is also considered a beneficial
gut bacterium. Thus, there is a chance that too much yogurt
MIGHT be detrimental.
REFERENCE 1: Yogurt Support
REFERENCE 2: Yogurt Support
REFERENCE 3: Yogurt Decreases Odoribacter Bacterium
CAUTION: Not all yogurts are made the same; therefore, some yogurt brands
MIGHT be more beneficial than others.
Most yogurt studies do NOT include the brand of the yogurt used,
and they don't compare one yogurt brand to another.
They also don't identify the starter bacteria (Lactobacillus
Bulgaricus, Streptococcus Thermophilus,
Bifidobacterium Lactis or Lactobacillus Acidophilus) that were used
to start the yogurt; therefore, the specific probiotics that are
produced by the yogurt is not known.
Starter bacteria are the bacteria that are used to cause
fermentation of the yogurt, and they can vary.
Starter bacteria include the following:
Lactobacillus Bulgaricus, Streptococcus Thermophilus,
Bifidobacterium Lactis or Lactobacillus Acidophilus.
The starter bacteria determine
the probiotics
that are produced at the end of the fermentation process.
Generally, yogurts labeled "Live Active Culture" are
considered to have more probiotics. A couple of the brands
that meet this criteria are the following:
Chobani, Activia, Stonyfield, FAGE, and Siggi's.
But, there are no studies
that prove one yogurt brand is better than the other.
3. Plantains

There was a study on one specific food, called plantains
and c diff. In the study, plantains were
found to both inhibit c diff and decrease
the ability of c diff bacteria to stick to the wall of the intestines.
CAUTION: This study was ONLY DONE in the laboratory;
thus, the effect on eating plantains by humans
is unknown.
Reference: Plantain Are Beneficial
Reference: Plantain Supplement
DIET SUMMARY
A diet for C diff is COMPLICATED.
It needs to be INDIVIDUALIZED and adjusted over time.
In addition, there are no tests available to determine if
a person is eating the right foods to attain the ideal
gut microbiome.
There are NO foods or diets that are definitely helpful
because there are no studies that have determined
what the ideal gut microbiomes are, and there are no
tests that an individual can do to determine if they are
moving toward the perfect gut microbiome. (There is a
GI Panel Test available, which tests about 40 gut bacteria,
but there are over 500 gut bacteria, and the GI Panel test
only test for about 40.)
Because of these difference, there are a variety of
diet suggestions.
EACH PERSON MUST CONSIDER THEIR OWN CIRCUMSTANCES
BEFORE MAKING ADJUSTMENT TO THEIR DIET.
Lastly, it must be mentioned that a person might NOT NEED
to alter their diet at all.
1. A person could choose to simply take the antibiotics for
c diff and eat a regular diet.
This works for some people.
2. A person could choose to take medications that are used
for Irritable Bowel Syndrome and eat a regular diet.
Medications for IBS are medications such as Bentyl, Imodium,
Elavil, and Nortriptyline. These work for some people--but
they OFTEN have side effects.
3. A person could try a variety of supplements and
continue to eat their regular diet.
These supplements include, but are not limited to
Florastor, Bentonite Clay, and Black Seed Oil.
These treatments also sometimes work.
They are explained in another section
of this website.
CAUTION ON ALL DIET INFORMATION
Before anyone adjusts their diets,
they should be aware that there
are four problems with the studies that have been done.
The first problem is that rodents and humans
have vastly different intestines.
Not only is the shape of rodents’ intestines different,
but rodents have different normal gut bacteria.
The second problem is that the only study that was done on people
was done on HEALTHY people NOT people who are
infected with c diff. A person who is infected
with c diff and has an inflamed or irritated colon
MIGHT NOT respond the same way as a healthy person does.
The third problem is that laboratory studies (in vitro) have no
test on living organism; therefore, their applicability to people
infected with c diff is even more distant than the relationship
between mice and humans.
The fourth problem is that there are
conflicting reports between different studies.
These problems within these studies does NOT mean they should
be totally disregarded, but it does mean that they can
NOT be TOTALLY RELIED UPON.
REFERENCE: Protein Supplements to do NOT Help heal the intestines
A study compared a high-fat (low-fiber) diet to a
low-fat (low-fiber) diet on mice who had been infected with c diff.
1. High-fat (low-fiber) was called the Western Diet
2. Low-fat (low-fiber) = LF/LF Diet
The mice fed the Western Diet had a significantly higher death rate than
the LF/LF Diet.
A second study examined how a high-fat/high-protein diet (like the Atkins
Diet) increased the chance of c diff mortality by decreasing protective
bacteria (Lachnospiraceae and Ruminococcaceae).
This study compared three different diets:
1. high-fat/high-protein diet
2. high-fat/low-protein diet
3. carbohydrate/low-fiber diet.
Both of the high-fat diets
increased the chance of c diff mortality. The high-fat/high-protein diet
did it consitently; where as, the high-fat/low-protein diet had
mixed results.
The carbohydrate/low-fiber diet had the least
amount of illness.
REFERENCE: A High-Fat/High-Protein
Diet Increase C diff
A general population study empphasized the
potential harm of excessive fat intake.
However, this study was NOT specific to c diff.
It found that there was approximately a 5% increase in
deaths due to the consumption of excess dietary fat.
This was a meta analysis of 19 different studies. This meta analysis
contained over a million people in it and was conducted over
many years.
It demonstrated an association of a high-fat diet with
several illness, primarily cardiovascular disease and
cancers.
Caution: The total suggested dietary-fat for a day should be
about 20-35% of a person's total calorie count.
A minumum suggested amount of fat each
day is 20% of total daily calories.
Too little dietary fat, just like too much dietary fat
can also be detrimental.
High-Fat/Low-Fiber Increase Morality REFERENCE

4. Don't Eat A High-Calcium Diet
There is a study that found that feeding mice a calcium-deprived diet
reduced the c diff relapse in mice by 90%. The study found that calcium
is a necessary mineral needed for c diff to germinate (in mice).
CAUTION: It is important to remember the humans need a certain
amount of calcium in there diet, primarily to have strong bones;
however, they rarely need calcium supplements, and they are able
to go without
calcium foods for a period of time without reprocussions.
This study infers that if a person is at a
high risk for a c diff infection, that person MIGHT try
decreasing their calcium intake for a short period of time
to prevent relapsing.
However, it should always be remembered that this study was on mice,
and mice are vastly different from humans.
Not all results from mice studies hold true to people.
REFERENCE: Calcium-Deprived Diet
5. Don't Eat a High-Sugar Diet
A mice study found that
mice fed a VERY high-sucrose diet significantly increased their
mortality rate. The mice were fed a diet that contained 94% sucrose
(table sugar),
and the rest was from cornstarch and maltodextrin.
Caution: The
above study fed mice a diet that was 94% sucrose (table sugar).
The typical American diet has approximately 10-13% simple sugar.
The world
Health Association states that up 10% of a person's
daily calorie intake can be in the form of simple sugars, such
as table sugar. However, there is NO MINIMUM requirement
for the intake of simple sugars. A person can easily live
without the intake of simple sugar.
REFERENCE: A High-Sugar Diet is Bad
6. Don't Eat Excessive Salt

One study that found that
high-salt diets will decrease Lactobacillus Bacteria
(which is considered a good bacterium). Salt has also been
reported to cause c diff to
adhere to the colon wall better. Therefore, there is circumstantial
evidence that a high-salt diet MIGHT be detrimental to
a person trying to prevent c diff.
REFERENCE 1: Salt Decreases Good Gut Bacteria
REFERENCE 2: C diff Is Able to Adapt to High-Salt Environment
7. Don't Drink Excessive Alcohol
 One study on alchol abuse and c diff found
that if people abuse alcohol there is about a 2 fold risk of c diff
infection. However, the study subjects were
ALL known to be alcoholics, not just occasional alcohol drinkers.
Thus, there is some evidence
that drinking alcohol excessively will increase the risk
of c diff infection and
relapse, but there is no evidence that the same is true
for light-alcohol users.
One study on alchol abuse and c diff found
that if people abuse alcohol there is about a 2 fold risk of c diff
infection. However, the study subjects were
ALL known to be alcoholics, not just occasional alcohol drinkers.
Thus, there is some evidence
that drinking alcohol excessively will increase the risk
of c diff infection and
relapse, but there is no evidence that the same is true
for light-alcohol users.
However, there is also evidence that alcohol abuse is associated with
higher rates of inflammatory Bowel Disease (IBD). But,
once again, the studies indicate that there is a higher rate of
IBD among alcohol abuses, but don't define how much risk is
generated by drinking small amounts of alcohol.
REFERENCE:
Alcohol Increases Risk of C Diff
REFERENCE:
Alcohol Increases Risk of IBD
DOs
1. DO Consider a Low FODMAP Diet
During an infection with c diff, or immediately after
a c diff infection, many people will develop
post-infection irritable bowel syndrome (PI-IBS).
During this period of time
a person MIGHT need to follow a "Low" FODMAP diet
for a period of time. This period of time
is NOT clearly defined. It seems to vary between
a few weeks to many years. Ideally a low FODMAP diet
should NOT be followed for more than a couple of
months because eating a low FODMAP diet
can cause a decrease in a person's
good gut bacteria, which can inturn increase their
chance of c diff relapse.
FODMAP is an ancronym for for Fermentable Oligosaccharides,
Disaccharides, Monosaccharides, And Polyols.
These are short-chain carbohydrates that are
poorly absorbed in the small intestine and can
cause digestive issues
like gas, bloating, and diarrhea.
HOWEVER, these SAME
short-chain carbohydrates can increase the number
of good bacteria in the gut, and thereby decrease the
chance of c diff infection or relapse. Therefore,
while a LOW FODMAP diet MIGHT be necessary for some
period time after a person has c diff, it should not
be continued longer than it is necessary.
Low FODMAP foods are foods such as:
eggplant, green beans, bok choy, carrot, cucumber,
potato, oats, gluten free pasta, white rice, rice cakes,
sourdough bread, white bread, dark chocolate,
maple syrup, table sugar, eggs, firm tofu,
plain cooked meats, poultry and seafood.
REFERENCE: Low-FODMAP Diet for IBS
Caution: It is important to remember that some of the
food mentioned in a low-FODMAP diet are HIGH in protein
and some studies have indicated that a low protein/low fat
diet can reduce the chance of c diff relapse.
2. DO Consider an Elimination Diet
 If a person has Post Infection-Irritable Bowel Syndrome
and cannot tolerate the foods on the Low-FODMAP diet
they may want to consider an an "Elimination Diet."
An elimination diet is similar to the aforementioned Low-
FODMAP Diet, BUT is even more limited in the foods that
can be eaten. It also should not be continued any longer
than is absolutely necessary, because by eliminating
numerous foods a person can reduce the number of good
gut bacteria, which can be helpful to reduce the
chance of c diff infection.
If a person has Post Infection-Irritable Bowel Syndrome
and cannot tolerate the foods on the Low-FODMAP diet
they may want to consider an an "Elimination Diet."
An elimination diet is similar to the aforementioned Low-
FODMAP Diet, BUT is even more limited in the foods that
can be eaten. It also should not be continued any longer
than is absolutely necessary, because by eliminating
numerous foods a person can reduce the number of good
gut bacteria, which can be helpful to reduce the
chance of c diff infection.
There are two basic methods by which an elimination diet can
be done.
The first method is for a person to remove ALL the foods
from their diet that they
think are bothering them. After they are better
for a period time, they can test one additional new food
at a time to determine if they are able to tolerate the new food.
By increasing the diversity of their diet, they should
be able to increase the diveristy of the good bacteria in
their colon.
A second method of doing an elimination diet
is where ALL foods except either rice and
water or bread and water are removed.
After a period of time when their
gut feels reasonably well they start
testing one food at a time, watching each food for a reaction.
If a food can NOT be tolerated, then it should be temporarily eliminated.
Once a person feels better again, they can try a new food.
Each new food is usually tested for a couple of days before
testing another food. Foods that seem to cause a problem
can be retried when a person is
feeling better to determine if they are still intolerable.
REFERENCE: Elimination Diet for C Diff
3. DO Consider Eating Some Fermented Foods

The word "condsider" is used because some people
cannot tolerate fermented foods. In addition,
some fermented foods such as Yogurt and Kefir
contain high amount of calcium, which a person MIGHT
be trying to avoid after having c diff.
There was one small study, using 36 HEALTHY people, that studied how
fermented foods, "OR" a high-fiber diet influenced
the gut microbiome.
In this study, 36 subjects at Stanford were
grouped into one of two groups, one group ate a high-fiber diet,
and one group that ate a diet high in fermented
foods. All subjects were followed for 10 weeks.
The study found that
eating fermented foods three times a day
increased gut bacteria diversity, which in turn
reduced gut inflammatory markers. In contrast, the study also
found that eating a high-fiber diet for 10 weeks
did not change the gut bacteria.
REFERENCE: Fermented Food Reduces Gut Inflammation
Examples of Fermented Foods:
Kombucha (No Sugar Added)
Fermented Vegetables
Tempeh (Gluten-Free)
Miso (Refrigerated)
Pickles (In salt, Not vinegar)
Sauerkraut (Refrigerated)
Kimchi
Kefir
Plain Yogurt (Those marked Live Culture are probably better.)
Cottage Cheese (Those marked Live Culture are probably better.)
Certain aged cheeses (Check label for live and active cultures)
CAUTION: People with C diff were NOT used
for this study; therefore, the studies results MIGHT NOT
be APPLICABLE to people who have their intestines
inflamed or depleted of good intestinal bacteria due to a recent
c diff infection.
In addition, an increased diveristy of gut microbiomes does NOT
guarantee a person will have less c diff.
Lastly, one study found that eating yogurt increased
streptococcus bacteria--
but, at the same time decreased odoribacter bacteria.
The odoribacter bacteria is also considered to be
a good gut bacteria.
Thus, the overall benefit of eating yogurt
might not be as good as hoped.
REFERENCE: Eating Yogurt Decreases Odoribacter Bacteria
4. DO Consider Eating High-FODMAP Foods

The word "consider" is used because after a person has
had c diff, there intestines are oftentimes more sensitive
to all different types of foods, especially FODMAP foods.
However, FODMAPS foods are high in soluble fiber
and a diet high in soluble fiber has been found
to be protective against c diff.
If a person does not have PI-IBS and wants
to try to diversify their gut bacteria,
they can try to eat to some of the following FODMAP foods.
Oatmeal Cereal, peas, beans, apples,
bananas, avocados, citrus fruits, carrots, barley and psyllium.
Fiber Chart
A mice study found that mice that were fed a high-
soluble-fiber diet
produced MORE ACETATE in their intestine.
This increase in acetate helped regulate the immune response in
the protective layer of the colon. This in turn
was found to help protect against c diff.
REFERENCE: A High-Soluble-Fiber Diet Improves the
Immune System in Mice
CAUTION: A small study on humans found that
humans who ate a high-fiber diet for 10 weeks were unable to
change their intestinal bacteria.
5. DO Consider Eating Some Fruit (Apples, Oranges, Lemons, Berries)
Apples, oranges, lemons, and berries contain pectin and this pectin
has been found to be beneficial.
A study on mice found that the pectin helped
to improve intestinal integrity and
increase Lachnospiraceae bacteria in the intestine. Higher levels of
Lachnospiraceae bacteria are associated with better health.
MACs Reduce C diff in Mice Reference
Reference: Pectin
Might Decrease C diff in Mice
CAUTION: Fruits are FODMAP foods; therefore, if
a person has IBS or PI-IBS these foods may be hard to tolerate.
6. Do Drink Sufficient Water
Some people may decrease their fluid intake
to try minimize their diarrhea.
However, when a person is having loose bowel movements
or diarrhea they have
an increased chance to become dehydrated.
When a person is dehydrated they will often
not feel well; however, beyond not feeling well
being dehydrated can in some cases lead to kidney
damage and in extreme cases dehydration can cause death.
The average amount of fluids a person should drink in
a day is 1500 ml. 1500 ml is equal to 50 ounces of fluid,
or approximately three 500 ml bottles or water, or six
8 ounce glasses of water. However, if a person has diarrhea,
there if often a need for even more fluid.
In the worst case of dehydration, a person may need to get
fluids intravenously.
Caution: While being correctly hydrated is very important
to good health, excess fluids can be a problem as well.
Although, overhydration does not occur that often it can
cause excessive urination and a lowered sodium in the blood.
The lowered sodium is called hyponatremia, and it will also
cause a person feel poorly.
In addition, a person MUST be cautious when hydrating themselves.
Some electrolyte solutions such as Gatorade and Powerade
can actually cause diarrhea. It is best to try to hydrate
with a solution that contains a little salt and sugar. A person
can make their own or by Pedialyte.
SPECIFIC FOODS
1. Kefir

There is one study that reported that Kefir will favorably
change the gut microbiome.
Kefir was found to primarily increase Acetinobacteria.
Acetinobacteria is thought to
be a bacterium that is beneficial to the gut. It is hoped that
an increase in acetinobateria will
inhibit the growth of c diff spores.
CAUTION: The study that was done
only proved that kefir increase acetinobacteria,
it did not prove this increase
in acetinobacteria would decrease the rate of c diff infection or relapse.
Reference: Kefir
2. Yogurt

Yogurt probably has some short-term benefits on the
gut microbiomes.
A study has reported that a short-term increase in
Streptococcus Thermophilus and Bifidobacterium Animalis bacteria
among people eating yogurt.
These two bacteria are considered to be good gut bacteria.
However, another study found that was while they found an increase
in Streptococcus bacteria among regular yogurt eaters, it also found
a decrease in odoribacter bacteria. This odoribacter bacteria
is also considered a beneficial
gut bacterium. Thus, there is a chance that too much yogurt
MIGHT be detrimental.
REFERENCE 1: Yogurt Support
REFERENCE 2: Yogurt Support
REFERENCE 3: Yogurt Decreases Odoribacter Bacterium
CAUTION: Not all yogurts are made the same; therefore, some yogurt brands
MIGHT be more beneficial than others.
Most yogurt studies do NOT include the brand of the yogurt used,
and they don't compare one yogurt brand to another.
They also don't identify the starter bacteria (Lactobacillus
Bulgaricus, Streptococcus Thermophilus,
Bifidobacterium Lactis or Lactobacillus Acidophilus) that were used
to start the yogurt; therefore, the specific probiotics that are
produced by the yogurt is not known.
Starter bacteria are the bacteria that are used to cause
fermentation of the yogurt, and they can vary.
Starter bacteria include the following:
Lactobacillus Bulgaricus, Streptococcus Thermophilus,
Bifidobacterium Lactis or Lactobacillus Acidophilus.
The starter bacteria determine
the probiotics
that are produced at the end of the fermentation process.
Generally, yogurts labeled "Live Active Culture" are
considered to have more probiotics. A couple of the brands
that meet this criteria are the following:
Chobani, Activia, Stonyfield, FAGE, and Siggi's.
But, there are no studies
that prove one yogurt brand is better than the other.
3. Plantains

There was a study on one specific food, called plantains
and c diff. In the study, plantains were
found to both inhibit c diff and decrease
the ability of c diff bacteria to stick to the wall of the intestines.
CAUTION: This study was ONLY DONE in the laboratory;
thus, the effect on eating plantains by humans
is unknown.
Reference: Plantain Are Beneficial
Reference: Plantain Supplement
DIET SUMMARY
A diet for C diff is COMPLICATED.
It needs to be INDIVIDUALIZED and adjusted over time.
In addition, there are no tests available to determine if
a person is eating the right foods to attain the ideal
gut microbiome.
There are NO foods or diets that are definitely helpful
because there are no studies that have determined
what the ideal gut microbiomes are, and there are no
tests that an individual can do to determine if they are
moving toward the perfect gut microbiome. (There is a
GI Panel Test available, which tests about 40 gut bacteria,
but there are over 500 gut bacteria, and the GI Panel test
only test for about 40.)
Because of these difference, there are a variety of
diet suggestions.
EACH PERSON MUST CONSIDER THEIR OWN CIRCUMSTANCES
BEFORE MAKING ADJUSTMENT TO THEIR DIET.
Lastly, it must be mentioned that a person might NOT NEED
to alter their diet at all.
1. A person could choose to simply take the antibiotics for
c diff and eat a regular diet.
This works for some people.
2. A person could choose to take medications that are used
for Irritable Bowel Syndrome and eat a regular diet.
Medications for IBS are medications such as Bentyl, Imodium,
Elavil, and Nortriptyline. These work for some people--but
they OFTEN have side effects.
3. A person could try a variety of supplements and
continue to eat their regular diet.
These supplements include, but are not limited to
Florastor, Bentonite Clay, and Black Seed Oil.
These treatments also sometimes work.
They are explained in another section
of this website.
CAUTION ON ALL DIET INFORMATION
Before anyone adjusts their diets,
they should be aware that there
are four problems with the studies that have been done.
The first problem is that rodents and humans
have vastly different intestines.
Not only is the shape of rodents’ intestines different,
but rodents have different normal gut bacteria.
The second problem is that the only study that was done on people
was done on HEALTHY people NOT people who are
infected with c diff. A person who is infected
with c diff and has an inflamed or irritated colon
MIGHT NOT respond the same way as a healthy person does.
The third problem is that laboratory studies (in vitro) have no
test on living organism; therefore, their applicability to people
infected with c diff is even more distant than the relationship
between mice and humans.
The fourth problem is that there are
conflicting reports between different studies.
These problems within these studies does NOT mean they should
be totally disregarded, but it does mean that they can
NOT be TOTALLY RELIED UPON.
Caution: The total suggested dietary-fat for a day should be about 20-35% of a person's total calorie count. A minumum suggested amount of fat each day is 20% of total daily calories. Too little dietary fat, just like too much dietary fat can also be detrimental.
REFERENCE: Calcium-Deprived Diet
REFERENCE 1: Salt Decreases Good Gut Bacteria
REFERENCE 2: C diff Is Able to Adapt to High-Salt Environment
 One study on alchol abuse and c diff found
that if people abuse alcohol there is about a 2 fold risk of c diff
infection. However, the study subjects were
ALL known to be alcoholics, not just occasional alcohol drinkers.
Thus, there is some evidence
that drinking alcohol excessively will increase the risk
of c diff infection and
relapse, but there is no evidence that the same is true
for light-alcohol users.
One study on alchol abuse and c diff found
that if people abuse alcohol there is about a 2 fold risk of c diff
infection. However, the study subjects were
ALL known to be alcoholics, not just occasional alcohol drinkers.
Thus, there is some evidence
that drinking alcohol excessively will increase the risk
of c diff infection and
relapse, but there is no evidence that the same is true
for light-alcohol users.
However, there is also evidence that alcohol abuse is associated with higher rates of inflammatory Bowel Disease (IBD). But, once again, the studies indicate that there is a higher rate of IBD among alcohol abuses, but don't define how much risk is generated by drinking small amounts of alcohol.
REFERENCE: Alcohol Increases Risk of C Diff
REFERENCE: Alcohol Increases Risk of IBD
During an infection with c diff, or immediately after a c diff infection, many people will develop post-infection irritable bowel syndrome (PI-IBS). During this period of time a person MIGHT need to follow a "Low" FODMAP diet for a period of time. This period of time is NOT clearly defined. It seems to vary between a few weeks to many years. Ideally a low FODMAP diet should NOT be followed for more than a couple of months because eating a low FODMAP diet can cause a decrease in a person's good gut bacteria, which can inturn increase their chance of c diff relapse.
FODMAP is an ancronym for for Fermentable Oligosaccharides, Disaccharides, Monosaccharides, And Polyols. These are short-chain carbohydrates that are poorly absorbed in the small intestine and can cause digestive issues like gas, bloating, and diarrhea. HOWEVER, these SAME short-chain carbohydrates can increase the number of good bacteria in the gut, and thereby decrease the chance of c diff infection or relapse. Therefore, while a LOW FODMAP diet MIGHT be necessary for some period time after a person has c diff, it should not be continued longer than it is necessary.
Low FODMAP foods are foods such as:
eggplant, green beans, bok choy, carrot, cucumber, potato, oats, gluten free pasta, white rice, rice cakes, sourdough bread, white bread, dark chocolate, maple syrup, table sugar, eggs, firm tofu, plain cooked meats, poultry and seafood.
REFERENCE: Low-FODMAP Diet for IBS
 If a person has Post Infection-Irritable Bowel Syndrome
and cannot tolerate the foods on the Low-FODMAP diet
they may want to consider an an "Elimination Diet."
An elimination diet is similar to the aforementioned Low-
FODMAP Diet, BUT is even more limited in the foods that
can be eaten. It also should not be continued any longer
than is absolutely necessary, because by eliminating
numerous foods a person can reduce the number of good
gut bacteria, which can be helpful to reduce the
chance of c diff infection.
If a person has Post Infection-Irritable Bowel Syndrome
and cannot tolerate the foods on the Low-FODMAP diet
they may want to consider an an "Elimination Diet."
An elimination diet is similar to the aforementioned Low-
FODMAP Diet, BUT is even more limited in the foods that
can be eaten. It also should not be continued any longer
than is absolutely necessary, because by eliminating
numerous foods a person can reduce the number of good
gut bacteria, which can be helpful to reduce the
chance of c diff infection.
There are two basic methods by which an elimination diet can be done. The first method is for a person to remove ALL the foods from their diet that they think are bothering them. After they are better for a period time, they can test one additional new food at a time to determine if they are able to tolerate the new food. By increasing the diversity of their diet, they should be able to increase the diveristy of the good bacteria in their colon.
A second method of doing an elimination diet is where ALL foods except either rice and water or bread and water are removed. After a period of time when their gut feels reasonably well they start testing one food at a time, watching each food for a reaction. If a food can NOT be tolerated, then it should be temporarily eliminated. Once a person feels better again, they can try a new food. Each new food is usually tested for a couple of days before testing another food. Foods that seem to cause a problem can be retried when a person is feeling better to determine if they are still intolerable.
REFERENCE: Elimination Diet for C Diff

The word "condsider" is used because some people
cannot tolerate fermented foods. In addition,
some fermented foods such as Yogurt and Kefir
contain high amount of calcium, which a person MIGHT
be trying to avoid after having c diff.
There was one small study, using 36 HEALTHY people, that studied how
fermented foods, "OR" a high-fiber diet influenced
the gut microbiome.
In this study, 36 subjects at Stanford were
grouped into one of two groups, one group ate a high-fiber diet,
and one group that ate a diet high in fermented
foods. All subjects were followed for 10 weeks.
The study found that
eating fermented foods three times a day
increased gut bacteria diversity, which in turn
reduced gut inflammatory markers. In contrast, the study also
found that eating a high-fiber diet for 10 weeks
did not change the gut bacteria.
REFERENCE: Fermented Food Reduces Gut Inflammation
Examples of Fermented Foods:
Kombucha (No Sugar Added)
Fermented Vegetables
Tempeh (Gluten-Free)
Miso (Refrigerated)
Pickles (In salt, Not vinegar)
Sauerkraut (Refrigerated)
Kimchi
Kefir
Plain Yogurt (Those marked Live Culture are probably better.)
Cottage Cheese (Those marked Live Culture are probably better.)
Certain aged cheeses (Check label for live and active cultures)
CAUTION: People with C diff were NOT used
for this study; therefore, the studies results MIGHT NOT
be APPLICABLE to people who have their intestines
inflamed or depleted of good intestinal bacteria due to a recent
c diff infection.
In addition, an increased diveristy of gut microbiomes does NOT
guarantee a person will have less c diff.
Lastly, one study found that eating yogurt increased
streptococcus bacteria--
but, at the same time decreased odoribacter bacteria.
The odoribacter bacteria is also considered to be
a good gut bacteria.
Thus, the overall benefit of eating yogurt
might not be as good as hoped.
REFERENCE: Eating Yogurt Decreases Odoribacter Bacteria
4. DO Consider Eating High-FODMAP Foods

The word "consider" is used because after a person has
had c diff, there intestines are oftentimes more sensitive
to all different types of foods, especially FODMAP foods.
However, FODMAPS foods are high in soluble fiber
and a diet high in soluble fiber has been found
to be protective against c diff.
If a person does not have PI-IBS and wants
to try to diversify their gut bacteria,
they can try to eat to some of the following FODMAP foods.
Oatmeal Cereal, peas, beans, apples,
bananas, avocados, citrus fruits, carrots, barley and psyllium.
Fiber Chart
A mice study found that mice that were fed a high-
soluble-fiber diet
produced MORE ACETATE in their intestine.
This increase in acetate helped regulate the immune response in
the protective layer of the colon. This in turn
was found to help protect against c diff.
REFERENCE: A High-Soluble-Fiber Diet Improves the
Immune System in Mice
CAUTION: A small study on humans found that
humans who ate a high-fiber diet for 10 weeks were unable to
change their intestinal bacteria.
5. DO Consider Eating Some Fruit (Apples, Oranges, Lemons, Berries)
Apples, oranges, lemons, and berries contain pectin and this pectin
has been found to be beneficial.
A study on mice found that the pectin helped
to improve intestinal integrity and
increase Lachnospiraceae bacteria in the intestine. Higher levels of
Lachnospiraceae bacteria are associated with better health.
MACs Reduce C diff in Mice Reference
Reference: Pectin
Might Decrease C diff in Mice
CAUTION: Fruits are FODMAP foods; therefore, if
a person has IBS or PI-IBS these foods may be hard to tolerate.
6. Do Drink Sufficient Water
Some people may decrease their fluid intake
to try minimize their diarrhea.
However, when a person is having loose bowel movements
or diarrhea they have
an increased chance to become dehydrated.
When a person is dehydrated they will often
not feel well; however, beyond not feeling well
being dehydrated can in some cases lead to kidney
damage and in extreme cases dehydration can cause death.
The average amount of fluids a person should drink in
a day is 1500 ml. 1500 ml is equal to 50 ounces of fluid,
or approximately three 500 ml bottles or water, or six
8 ounce glasses of water. However, if a person has diarrhea,
there if often a need for even more fluid.
In the worst case of dehydration, a person may need to get
fluids intravenously.
Caution: While being correctly hydrated is very important
to good health, excess fluids can be a problem as well.
Although, overhydration does not occur that often it can
cause excessive urination and a lowered sodium in the blood.
The lowered sodium is called hyponatremia, and it will also
cause a person feel poorly.
In addition, a person MUST be cautious when hydrating themselves.
Some electrolyte solutions such as Gatorade and Powerade
can actually cause diarrhea. It is best to try to hydrate
with a solution that contains a little salt and sugar. A person
can make their own or by Pedialyte.
SPECIFIC FOODS
1. Kefir

There is one study that reported that Kefir will favorably
change the gut microbiome.
Kefir was found to primarily increase Acetinobacteria.
Acetinobacteria is thought to
be a bacterium that is beneficial to the gut. It is hoped that
an increase in acetinobateria will
inhibit the growth of c diff spores.
CAUTION: The study that was done
only proved that kefir increase acetinobacteria,
it did not prove this increase
in acetinobacteria would decrease the rate of c diff infection or relapse.
Reference: Kefir
2. Yogurt

Yogurt probably has some short-term benefits on the
gut microbiomes.
A study has reported that a short-term increase in
Streptococcus Thermophilus and Bifidobacterium Animalis bacteria
among people eating yogurt.
These two bacteria are considered to be good gut bacteria.
However, another study found that was while they found an increase
in Streptococcus bacteria among regular yogurt eaters, it also found
a decrease in odoribacter bacteria. This odoribacter bacteria
is also considered a beneficial
gut bacterium. Thus, there is a chance that too much yogurt
MIGHT be detrimental.
REFERENCE 1: Yogurt Support
REFERENCE 2: Yogurt Support
REFERENCE 3: Yogurt Decreases Odoribacter Bacterium
CAUTION: Not all yogurts are made the same; therefore, some yogurt brands
MIGHT be more beneficial than others.
Most yogurt studies do NOT include the brand of the yogurt used,
and they don't compare one yogurt brand to another.
They also don't identify the starter bacteria (Lactobacillus
Bulgaricus, Streptococcus Thermophilus,
Bifidobacterium Lactis or Lactobacillus Acidophilus) that were used
to start the yogurt; therefore, the specific probiotics that are
produced by the yogurt is not known.
Starter bacteria are the bacteria that are used to cause
fermentation of the yogurt, and they can vary.
Starter bacteria include the following:
Lactobacillus Bulgaricus, Streptococcus Thermophilus,
Bifidobacterium Lactis or Lactobacillus Acidophilus.
The starter bacteria determine
the probiotics
that are produced at the end of the fermentation process.
Generally, yogurts labeled "Live Active Culture" are
considered to have more probiotics. A couple of the brands
that meet this criteria are the following:
Chobani, Activia, Stonyfield, FAGE, and Siggi's.
But, there are no studies
that prove one yogurt brand is better than the other.
3. Plantains

There was a study on one specific food, called plantains
and c diff. In the study, plantains were
found to both inhibit c diff and decrease
the ability of c diff bacteria to stick to the wall of the intestines.
CAUTION: This study was ONLY DONE in the laboratory;
thus, the effect on eating plantains by humans
is unknown.
Reference: Plantain Are Beneficial
Reference: Plantain Supplement
DIET SUMMARY
A diet for C diff is COMPLICATED.
It needs to be INDIVIDUALIZED and adjusted over time.
In addition, there are no tests available to determine if
a person is eating the right foods to attain the ideal
gut microbiome.
There are NO foods or diets that are definitely helpful
because there are no studies that have determined
what the ideal gut microbiomes are, and there are no
tests that an individual can do to determine if they are
moving toward the perfect gut microbiome. (There is a
GI Panel Test available, which tests about 40 gut bacteria,
but there are over 500 gut bacteria, and the GI Panel test
only test for about 40.)
Because of these difference, there are a variety of
diet suggestions.
EACH PERSON MUST CONSIDER THEIR OWN CIRCUMSTANCES
BEFORE MAKING ADJUSTMENT TO THEIR DIET.
Lastly, it must be mentioned that a person might NOT NEED
to alter their diet at all.
1. A person could choose to simply take the antibiotics for
c diff and eat a regular diet.
This works for some people.
2. A person could choose to take medications that are used
for Irritable Bowel Syndrome and eat a regular diet.
Medications for IBS are medications such as Bentyl, Imodium,
Elavil, and Nortriptyline. These work for some people--but
they OFTEN have side effects.
3. A person could try a variety of supplements and
continue to eat their regular diet.
These supplements include, but are not limited to
Florastor, Bentonite Clay, and Black Seed Oil.
These treatments also sometimes work.
They are explained in another section
of this website.
CAUTION ON ALL DIET INFORMATION
Before anyone adjusts their diets,
they should be aware that there
are four problems with the studies that have been done.
The first problem is that rodents and humans
have vastly different intestines.
Not only is the shape of rodents’ intestines different,
but rodents have different normal gut bacteria.
The second problem is that the only study that was done on people
was done on HEALTHY people NOT people who are
infected with c diff. A person who is infected
with c diff and has an inflamed or irritated colon
MIGHT NOT respond the same way as a healthy person does.
The third problem is that laboratory studies (in vitro) have no
test on living organism; therefore, their applicability to people
infected with c diff is even more distant than the relationship
between mice and humans.
The fourth problem is that there are
conflicting reports between different studies.
These problems within these studies does NOT mean they should
be totally disregarded, but it does mean that they can
NOT be TOTALLY RELIED UPON.
In addition, an increased diveristy of gut microbiomes does NOT guarantee a person will have less c diff.
Lastly, one study found that eating yogurt increased streptococcus bacteria-- but, at the same time decreased odoribacter bacteria. The odoribacter bacteria is also considered to be a good gut bacteria. Thus, the overall benefit of eating yogurt might not be as good as hoped.
Oatmeal Cereal, peas, beans, apples, bananas, avocados, citrus fruits, carrots, barley and psyllium.
Fiber Chart
A mice study found that mice that were fed a high- soluble-fiber diet produced MORE ACETATE in their intestine. This increase in acetate helped regulate the immune response in the protective layer of the colon. This in turn was found to help protect against c diff.
REFERENCE: A High-Soluble-Fiber Diet Improves the Immune System in Mice
MACs Reduce C diff in Mice Reference
Reference: Pectin Might Decrease C diff in Mice
The average amount of fluids a person should drink in a day is 1500 ml. 1500 ml is equal to 50 ounces of fluid, or approximately three 500 ml bottles or water, or six 8 ounce glasses of water. However, if a person has diarrhea, there if often a need for even more fluid.
In the worst case of dehydration, a person may need to get fluids intravenously.
In addition, a person MUST be cautious when hydrating themselves. Some electrolyte solutions such as Gatorade and Powerade can actually cause diarrhea. It is best to try to hydrate with a solution that contains a little salt and sugar. A person can make their own or by Pedialyte.
Reference: Kefir
However, another study found that was while they found an increase in Streptococcus bacteria among regular yogurt eaters, it also found a decrease in odoribacter bacteria. This odoribacter bacteria is also considered a beneficial gut bacterium. Thus, there is a chance that too much yogurt MIGHT be detrimental.
REFERENCE 1: Yogurt Support
REFERENCE 2: Yogurt Support
REFERENCE 3: Yogurt Decreases Odoribacter Bacterium
Generally, yogurts labeled "Live Active Culture" are considered to have more probiotics. A couple of the brands that meet this criteria are the following: Chobani, Activia, Stonyfield, FAGE, and Siggi's. But, there are no studies that prove one yogurt brand is better than the other.
CAUTION: This study was ONLY DONE in the laboratory; thus, the effect on eating plantains by humans is unknown.
There are NO foods or diets that are definitely helpful because there are no studies that have determined what the ideal gut microbiomes are, and there are no tests that an individual can do to determine if they are moving toward the perfect gut microbiome. (There is a GI Panel Test available, which tests about 40 gut bacteria, but there are over 500 gut bacteria, and the GI Panel test only test for about 40.)
Because of these difference, there are a variety of diet suggestions. EACH PERSON MUST CONSIDER THEIR OWN CIRCUMSTANCES BEFORE MAKING ADJUSTMENT TO THEIR DIET.
Lastly, it must be mentioned that a person might NOT NEED to alter their diet at all.
1. A person could choose to simply take the antibiotics for c diff and eat a regular diet. This works for some people.
2. A person could choose to take medications that are used for Irritable Bowel Syndrome and eat a regular diet. Medications for IBS are medications such as Bentyl, Imodium, Elavil, and Nortriptyline. These work for some people--but they OFTEN have side effects.
3. A person could try a variety of supplements and continue to eat their regular diet. These supplements include, but are not limited to Florastor, Bentonite Clay, and Black Seed Oil. These treatments also sometimes work. They are explained in another section of this website.
Before anyone adjusts their diets, they should be aware that there are four problems with the studies that have been done.
The first problem is that rodents and humans have vastly different intestines. Not only is the shape of rodents’ intestines different, but rodents have different normal gut bacteria.
The second problem is that the only study that was done on people was done on HEALTHY people NOT people who are infected with c diff. A person who is infected with c diff and has an inflamed or irritated colon MIGHT NOT respond the same way as a healthy person does.
The third problem is that laboratory studies (in vitro) have no test on living organism; therefore, their applicability to people infected with c diff is even more distant than the relationship between mice and humans.
The fourth problem is that there are conflicting reports between different studies.
These problems within these studies does NOT mean they should be totally disregarded, but it does mean that they can NOT be TOTALLY RELIED UPON.
VI. What ARE NEW TREATMENTS BEING STUDIED?
*If you want to see if there are any new treatment studies
that are going on in the United States you can check the following
website, https://clinicaltrials.gov.
Click Here
1. VE303 (RESTORATiVE303)
 VE303 is one of the more promising new treatments for c diff.
It is a new type of FMT that is being tested and thus
far has been found to be about as effective as Vowst.
However, this type of FMT is different from Vowst because
VE303 it is NOT made from human excrement. Vowst is.
Instead, VE303 is
made from 8 specific bacteria, which are grown in a
laboratory. The advantage of VE303 over Vowst is that
there is less risk of adverse effects. This treatment is
currently in Phase 3 and is looking for participants.
VE303 is one of the more promising new treatments for c diff.
It is a new type of FMT that is being tested and thus
far has been found to be about as effective as Vowst.
However, this type of FMT is different from Vowst because
VE303 it is NOT made from human excrement. Vowst is.
Instead, VE303 is
made from 8 specific bacteria, which are grown in a
laboratory. The advantage of VE303 over Vowst is that
there is less risk of adverse effects. This treatment is
currently in Phase 3 and is looking for participants.
Phase 3 Study Looking for Particpants
2. DAV132

DAV132 is an enteric-coated activated charcoal.
Enteric coated means it has a hard outer shell designed to
prevent the pill from being broken down in the small intestines, but rather
being broken down in the large intestines. Once it is broken down in the
large intestines the activated charcoal will absorb unwanted antibiotics
while
preserving the good intestinal bacteria.
Two research studies have demonstrated
that it is partially effective, but further
research still needs to be done.
It is currently in phase 2 trials; But, the trials are being
conducted in France, Bulgaria, Serbia and France. There are none
in the United States.
3. Ebselen
Ebselen is a medication is currently being studied
for the treatment for Meniere's disease; however,
some researchers have also looked at it for the use
in treating c diff.
One study on mice showed that ebselen decreased
intestinal inflammation and damage due to c diff toxins.
The problem with this information, is the study was done on mice and
there are no studies currently being done on ebselen for the
purpose of treating c diff. There are studies researching
the effectiveness on Meniere's disease, cochlear implants,
and depression--but none regarding c diff.
Thus, the effectiveness on people who have c diff
has yet to be proven. Perhaps more information will be
gained on the effectiveness of ebselen for c diff through the other
investigational studies.
Reference 1: Ebselen for C diff
Reference 2: Ebselen for C diff
Reference 3: Ebselen for C diff
4. SYN-004 (Ribaximase)

SYN004 (ribaximase) is a medication designed to break down
beta-lactam antibiotics after they have entered the large intestines.
Beta-lactam antibiotics are
antibiotics such as penicillin, amoxicillin, Keflex and Rocephin.
One study reported that
ribaximase did reduce the percentage of people who got c diff while
taking it; however, the same study showed that those people
who received rebaximase had substantially more adverse effects. The
authors reported that they thought the adverse effects where
coincidental.
There is currently a study being conducted that may
determine the effectiveness and chance of adverse effects; but
the trial is in Missouri, and it is only on people who are receiving treatment
for a severe blood disease.
Reference: SYN004
VII. NON-CONVENTIONAL TREATMENTS :
1. SACCHAROMYCES BOULARDII
 Saccharomyces Boulardii
benefits are highly debated.
Florastor is a common brand of Saccharomyces Boulardii.
In theory, Saccharomyces boulardii (SB) should help reduce c diff
because SB has been found
to produce a protease which inactivates the receptor site for C.
difficile toxin A.
Saccharomyces Boulardii
benefits are highly debated.
Florastor is a common brand of Saccharomyces Boulardii.
In theory, Saccharomyces boulardii (SB) should help reduce c diff
because SB has been found
to produce a protease which inactivates the receptor site for C.
difficile toxin A.
Reference: Probiotics Debated
This theory is supported by a hospital study conducted in 2021
with over 8000 hospitalized patients.
This study, which gave patients 500 mg SB 2x/day,
found that giving saccharomyces boulardii reduced
the chance of c diff occurring from 0.82% to 0.56%.
Reference:Saccharmyces Boulardii Support
Another small study found that giving patients Saccharomyces Boulardii,
who were taking high doses of vancomycin (presumably 500 mg 4x/day),
reduced
their chance of c diff relapse. However, this was NOT found to be
true among
patients taking a lower dose of vancomycin
(presumably 125 mg
4x/day).
Reference: Reduced Evidence that Saccharomyces Boulardii Helps
In addition to the one study that did not find a benefit among
patients receiving low-dose vancomycin, some medical
doctors discourage the use of saccharomyces boulardii.
Among these doctors are Dr. Cynthia Sears, an infectious disease doctor,
and Dr Curtis Donsky, also an infectious disease doctor.
Dr Curtis tells his
patients that if they decide to take Sarchomyces Boularii,
they should probably only take it for 28 days.
These doctors do not specifically explain why they don't suggest
the use of Sarchomyces Boularii; however, it is known that
the use of Sarchomyces Boularii has a RARE risk of
fungal septicemia (fungemia).
Reference: Fungal Septicemia is Possible
Reference: MD States Limit Saccharomyces Boulardii to 28 Days
2. Bentonite Clay

Bentonite Clay has many positive articles written about it regarding the absorption
of toxins; however, few specifically associate bentonite clay
with the treatment of c diff.
However, there is one article that describes the combination of Bentonite Clay
with Black Seed oil and lactobacillus probiotics that reports that a 2-year-old
was cured of c diff with this combination.
Reference: Bentonite Clay

3. Black Seed Oil
There is some evidence that Black Seed Oil (2%) with myrrh
water can inhibit the growth
of c diff.
Reference: Black Seed Oil
In addition, there has been at least one documented case of
successfully treating
a 2-year-old child with a combination of bentonite clay,
black seed oil and lactobacillus probiotics.
Reference: Lactobacillus, Bentonite Clay, Black Seed Oil
4. BILE ACIDS REDUCTION WITH QUESTRAN (Cholestyramine: Questran)
It seems that at the time of c diff infection, for unknown reasons,
there is often a change in
both primary and secondary bile acids.
When primary bile acid enters the large intestine,
the primary bile acid is converted into over 50
different secondary bile acids.
If the ratio is unbalanced,
a person will often have less of the good gut bacteria.
This imbalance can also contribute to inflammation and diarrhea.
A small study (less than 50 people) found that people given
cholestyramine (Questran),
a bile acid sequestran (binder),
along with Rocephin IV (a strong antibiotic)
had a lower rate of getting c diff infection than those who did not.
Thus, cholestyramine (Questran) MIGHT have some
role in preventing or treating c diff.
Reference: Bile Sequestrant Support

5. Butyrate
Butyrate is a short-chain fatty acid (SCFA) produced by beneficial bacteria
in the gut.
It is
found primarily in beans, peas, soybeans, fruits, and nuts.
It may have a role in preventing and treating c diff because it helps
to regulate the balance between primary bile acid and secondary bile acids,
which tend to become unbalanced when a person has c diff.
It also has an anti-inflammatory effect.
A study on mice found that giving mice a supplement of butyrate helped to
regulate bile acid metabolism and reduce inflammation.
Reference: Butyrate Benefits

6. CBD (CANNABIDIOL)
CBD (cannabidiol), has also been shown to have some effect in reducing
the chance of getting c diff.
This was demonstrated in a retrospective study that examined
CBD users and non-CBD users who were hospitalized.
Reference: CBD Risk of C Diff
In addition, another study, which was done in the laboratory–not
with real people–
found that CBD helped a particular type of colon cells heal.
Reference: CBD Colon Cell
7. IVIG: Intravenous Immunoglobulin (IVIG)
 Intravenous Immunoglobulin (IVIG)
MIGHT be of some help for people who have a reduced immune system,
such as those who have recently had cancer.
One 72-year-old patient, who had recently received cancer
treatment and who also had recurring
c diff, was given one IVIG infusion and was able to stop his
recurring c diff. He was given one dose of 400 mg IVIG.
However, it should be remembered that IVIG is not a standard treatment
for c diff, and it is very expensive, about $10,000 for one treatment;
therefore, it is rarely ordered for average people who have c diff.
Intravenous Immunoglobulin (IVIG)
MIGHT be of some help for people who have a reduced immune system,
such as those who have recently had cancer.
One 72-year-old patient, who had recently received cancer
treatment and who also had recurring
c diff, was given one IVIG infusion and was able to stop his
recurring c diff. He was given one dose of 400 mg IVIG.
However, it should be remembered that IVIG is not a standard treatment
for c diff, and it is very expensive, about $10,000 for one treatment;
therefore, it is rarely ordered for average people who have c diff.
Reference: IVIG
 Oral Immunoglobulin IgG is a possible substitute for IV
immunoglobulin G,
and it is much less expensive. It costs
about $600 for 30 doses, a week’s worth. The oral form of
IgG is called Enteragam.
Although there are no specific
studies reporting that Enteragam reduces c diff infection,
there have been 2
case reports of Enteragam helping patients resolve IBS after they have had
c diff.
Oral Immunoglobulin IgG is a possible substitute for IV
immunoglobulin G,
and it is much less expensive. It costs
about $600 for 30 doses, a week’s worth. The oral form of
IgG is called Enteragam.
Although there are no specific
studies reporting that Enteragam reduces c diff infection,
there have been 2
case reports of Enteragam helping patients resolve IBS after they have had
c diff.
Reference: Enteragam Reduces PI-IBS
8. LACTOBACILLUS REUTERI
.png) One probiotic that has some evidence that it is helpful
is Lactobacillus Reuteri. According a laboratory study
lactobacillus reuteri a type of food called "Glycerol"
and forms
"reuterin." (Glycerol is an oil or fat found in food.)
The reuterin enters a c diff bacterium cell and
activates a "reactive oxygen system" ROS. This process
kills
a c diff bacterium cell.
One probiotic that has some evidence that it is helpful
is Lactobacillus Reuteri. According a laboratory study
lactobacillus reuteri a type of food called "Glycerol"
and forms
"reuterin." (Glycerol is an oil or fat found in food.)
The reuterin enters a c diff bacterium cell and
activates a "reactive oxygen system" ROS. This process
kills
a c diff bacterium cell.
Caution: This hypothesis was only tested in a laboratory.
It was NOT tested on either rodent or humans; therefore,
while
it MIGHT be true for a person, it can NOT be relied upon.
Reference: L. Reuteri Might Reduce C diff Infection
Video How To Make L. Reuteri Yogurt
9. LACTOBACILLUS PLANTARUM 299v
 One probiotic that has some evidence that it is helpful
is Lactobacillus Plantarum.
It was tried on 44 adult ICU patients in 2008.
This small study found that none of the 22 ICU patients who were
given fermented
oatmeal gruel containing
Lactobacillus Plantarum 299v got c diff.
However, 4 of the 22 ICU patients who did not get Lactobacillus
299v got c diff.
One probiotic that has some evidence that it is helpful
is Lactobacillus Plantarum.
It was tried on 44 adult ICU patients in 2008.
This small study found that none of the 22 ICU patients who were
given fermented
oatmeal gruel containing
Lactobacillus Plantarum 299v got c diff.
However, 4 of the 22 ICU patients who did not get Lactobacillus
299v got c diff.
Lactobacillus Plantarum 299V Reference
10. Melatonin
 There is a study that found that Veterans who took Melatonin
reduced their chance of having c diff. The theory
of why this happened is that Melatonin can decrease
inflammation, and a reduction in inflammation can decrease
relapse rates. This study was conducted on
patients at the VA Hospital. The study did NOT
disclose the dose of Melatonin used, however.
But, it is known that the usual dosage
recommended to treat inflammation is 10mg/day of melatonin.
This is a relatively high dose of melatonin, and it
may cause many people to be very sedated in the morning after taking it.
There is a study that found that Veterans who took Melatonin
reduced their chance of having c diff. The theory
of why this happened is that Melatonin can decrease
inflammation, and a reduction in inflammation can decrease
relapse rates. This study was conducted on
patients at the VA Hospital. The study did NOT
disclose the dose of Melatonin used, however.
But, it is known that the usual dosage
recommended to treat inflammation is 10mg/day of melatonin.
This is a relatively high dose of melatonin, and it
may cause many people to be very sedated in the morning after taking it.
Reference: Melatonin
11. METAMUCIL
 One 72-year-old man with recurrent c diff was told to take Metamucil
while waiting
for his newest c diff results. Remarkably, by the time his test
results came back positive, he
reported he no longer had symptoms. He was followed over the next
few months,
and his c diff did NOT recur.
One 72-year-old man with recurrent c diff was told to take Metamucil
while waiting
for his newest c diff results. Remarkably, by the time his test
results came back positive, he
reported he no longer had symptoms. He was followed over the next
few months,
and his c diff did NOT recur.
It is hypothesized that it was the fiber
in the Metamucil that helped him. However, other than this
one 72-year-old man,
there are no studies correlating Metamucil with the treatment of c diff.
But, there is some evidence that a high-fiber diet MIGHT
increase the good bacteria in the colon; therefore,
it is possible that Metamucil MIGHT have caused an
increase in good bacteria, and
thereby cured him.
However, to reiterate, it is uncertain whether Metamucil is
helpful for c diff patients or not.
Reference: 72-Year-Old-Man Cured with Metamucil
12. Manuka Honey (Enema)
 A manuka Honey enema MIGHT have some benefit in the treatment of C diff;
however, the evidence is very weak.
There was one 71-year-old male patient who had recurrent c diff
who was treated with
a Manuka Honey “ENEMA” and was reported cured of his c diff.
In addition, there are other studies
that show Manuka Honey has antimicrobial effects.
However, most of these studies
have been done in vitro. In vitro means that it was done
in a test tube, or a culture plate, and no animals
or humans were used.
There are no animal or human studies that have been done to
show that Manuka Honey
has an inhibitory effect
on patients with active c diff.
A manuka Honey enema MIGHT have some benefit in the treatment of C diff;
however, the evidence is very weak.
There was one 71-year-old male patient who had recurrent c diff
who was treated with
a Manuka Honey “ENEMA” and was reported cured of his c diff.
In addition, there are other studies
that show Manuka Honey has antimicrobial effects.
However, most of these studies
have been done in vitro. In vitro means that it was done
in a test tube, or a culture plate, and no animals
or humans were used.
There are no animal or human studies that have been done to
show that Manuka Honey
has an inhibitory effect
on patients with active c diff.
In fact, the authors of one in vitro study on Manuka Honey
were quoted as saying,
“...we did not find manuka honey to be universally bactericidal or
inhibitory against C. difficile growth...”
Reference: Manuka Honey Enema
Reference: Manuka Honey Variable Effects
Reference: No Universal Inhibitor Effects
13. Vitamin D
 A deficiency in vitamin D is associated with a 4.75 times higher risk of
dying from c diff.
A small study with 65 patients was conducted. Those who were
deficient in Vitamin D had poorer outcomes.
Vitamin D
deficiency was defined as having a blood vitamin D level less than 21 ng/dl.
If a person wants to increase their Vitamin D they have three choices. One
choice is to take a daily supplement of Vitamin (~2,000 IU).
A second way would be to sit in the sun for 10 minutes to 2 hours.
The less body parts that are exposed, the darker the skin, and the older
a person is, the MORE time they will need to be exposed to sunlight
each day. A third
way is to get an injection of vitamin each week. This injection
usually contains 50,000.
A deficiency in vitamin D is associated with a 4.75 times higher risk of
dying from c diff.
A small study with 65 patients was conducted. Those who were
deficient in Vitamin D had poorer outcomes.
Vitamin D
deficiency was defined as having a blood vitamin D level less than 21 ng/dl.
If a person wants to increase their Vitamin D they have three choices. One
choice is to take a daily supplement of Vitamin (~2,000 IU).
A second way would be to sit in the sun for 10 minutes to 2 hours.
The less body parts that are exposed, the darker the skin, and the older
a person is, the MORE time they will need to be exposed to sunlight
each day. A third
way is to get an injection of vitamin each week. This injection
usually contains 50,000.
Reference: Low Vitamin D Caused Poor
Outcomes
One other study found that administering a high dose of vitamin D increased the
good gut bacteria.
Reference: High Dose Vitamin D Increases Good Gut Bacteria
VII. THINGS THAT ARE PROBABLY BAD FOR C DIFF
 1. Certain antacids: Several studies have found that antacids
increase the chance of c diff infection, and at least one that was found
the opposite. Two studies found that stronger antacids (PPIs) such as:
1. Certain antacids: Several studies have found that antacids
increase the chance of c diff infection, and at least one that was found
the opposite. Two studies found that stronger antacids (PPIs) such as:
Prilosec (omeprazole),
Neximum (esomeprozole)
Protonix (Pataprazole)
Are PROBABLY the highest risk for increasing the chance of c diff.
Histamine Blockers (H2 Blockers) such as:
Cimetidine (Tagamet)
Famotidine (Pepcid)
Nizatidine (Axid)
Are also associated with c diff infection--but to a lesser degree (OR[odds ratio] of 1.96 compared to 1.40 respectively.
The theory of why c diff is associated with antacids is that the stomach's acidity helps to kill unwanted bacteria. If the stomach is less acidic, more harmful bacteria can occur. The good news is that the lower the dose and the shorter the duration these medications are used, the less likely they are to cause a c diff infection. One study found that if antacids were taken for less than 2 weeks, there was a very low chance of the antacid leading to c diff.
Reference 1: Antacid Increase Risk of C. Diff.
Reference 2: Antacid Increase Risk of C. Diff.
Reference 3: Antacid Don't Increase Risk of c diff
 3. Most Oral and Intravenous Antibiotics
3. Most Oral and Intravenous Antibiotics
Most antibiotics, whether or not they are taken orally or given intravenously, can cause c diff. Most people get c diff after taking antibiotics. One study found that only about 7% of c diff infections occur without people taking antibiotics.
Each antibiotic has its own risk of causing an infection. Rocephine, given intravenously, is probably the highest risk IV antibiotic. Clindamycin, Augmentin, and Amoxicillin are probably the highest risk oral antibiotics. Among the lowest risk antibiotics are Doxycycline, Macrobid and Gentamycin (given intramuscularly or intravenously).
Reference 1: Antibiotics
Reference 2: Antibiotics
Reference 3: Antibiotics
Reference 4: Antibiotics
 4. Trehalose
4. Trehalose
There was a study that indicated that trehalose MIGHT increase c diff virulence. Trehalose is a naturally occurring sugar found in shellfish, oysters, yeast, honey (primarily honey produce by stingless bees), and in many edible mushrooms, (including shiitake, oyster, king oyster, and golden needle mushrooms, yeast, , and shellfish.)
Reference: Trehalose
 5. High-Sugar Diet
5. High-Sugar Diet
A high-sugar diet is not directly associated with c diff, but it has been shown to increase proteobacteria in the gut, while simultaneously decreasing the abundance of Bacteroidetes, which can mitigate the effects of endotoxin, as well as reinforce gut barrier function. The result is more proinflammatory bacteria. However, it should be mentioned, that there are no studies on low-to-moderate-sugar diets that associate them with a negative microbiome change.
Reference: High-Sugar Diet Is Detrimental
 8. Indomethecin (High-Strength NSAIDS)
8. Indomethecin (High-Strength NSAIDS)
Indomethecin, which is a high-strength prescription NSAID (non-steroidal anti-inflammatory drug) has been found to be associated with a higher rate of deterioration among mice infected with c diff. This study found that mice given indometacin had more severe symptoms than those that didn't. A follow-up study found that indomethacin injured the upper layer of the intestinal wall, which the researchers suggested caused an increased susceptibility to c diff infection.
Reference 1: Indomethacin
Reference 2: Indomethacin
9. Oral Iron Supplements
 There are several causes of anemia. If anemia is due to a low level of iron,
and it is severe, it will probably require treatment with either Oral iron (pills)
or intravenous (IV) iron.
There are several causes of anemia. If anemia is due to a low level of iron,
and it is severe, it will probably require treatment with either Oral iron (pills)
or intravenous (IV) iron.
There has been at least one study that has found that taking oral iron MIGHT increase a person's chance of c diff relapse.
Reference: Iron Increases Chance of C. Diff.
However, there are no studies that have found an association between IV iron and c diff.
VIII. THINGS THAT COULD BE EITHER GOOD OR BAD FOR C DIFF
There have been several studies done on antidepressant and their association with c diff. Unfortunately, the studies have not reached the same results. One study found that only two antidepressants (Prozac [fluoxetine] and Remeron [mirtazapine]) increased the chance of c diff infection.
Another study found that the following antidepressant could increase the chance of c diff relapse.
Paxil (paroxetine)
Prozac (fluoxetine)
Remeron (mirtazapine)
Desyrel (trazodone)
 A third study found that a few antidepressants were
associated with either no risk or a lower risk of c diff.
A third study found that a few antidepressants were
associated with either no risk or a lower risk of c diff.
The antidepressants that were found to actually reduce the risk of c diff were the following:
Zoloft (sertraline)
Lexapro (escitalopram)
Celexa (citalopram).
Reference: High-Risk Antidepressant
Reference: Medium-Risk Antidepressant
2. Steroids (Cortisone Injection, Prednisone, Budesonide, etc.)
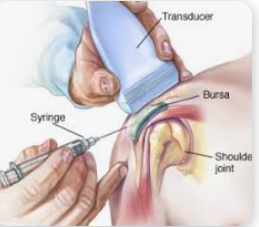 Steroids are debated in their risk and benefits.
There is a study that found that taking steroids reduced the
risk of c diff.
There is another study that found that taking steroids increased the risk of c diff.
These conflicting results make it difficult to know if steroids help or hinder c diff.
Whether steroids can decrease or increase c diff infection MIGHT
be due to the dose that is administered and the reason that it
is administered. No general statement can be made regarding the
use of steroids.
Steroids are debated in their risk and benefits.
There is a study that found that taking steroids reduced the
risk of c diff.
There is another study that found that taking steroids increased the risk of c diff.
These conflicting results make it difficult to know if steroids help or hinder c diff.
Whether steroids can decrease or increase c diff infection MIGHT
be due to the dose that is administered and the reason that it
is administered. No general statement can be made regarding the
use of steroids.
Reference: Steroid Support
Reference 1: Steroid Avoidance
Reference 2: Steroid Avoidance
3. OXYGEN THERAPY
 Oxygen therapy via a hyperbaric chamber MIGHT be of some benefit.
There are two studies regarding c diff and an oxygen increased environment via a hyperbaric chamber.
The study on human found hyperbaric oxygen treatment was beneficial, while the study on mice found no benefit
of hyperbaric oxygen on mice.
Oxygen therapy via a hyperbaric chamber MIGHT be of some benefit.
There are two studies regarding c diff and an oxygen increased environment via a hyperbaric chamber.
The study on human found hyperbaric oxygen treatment was beneficial, while the study on mice found no benefit
of hyperbaric oxygen on mice.
Reference 1: Oxygen
Reference 2: Oxygen
IX. THINGS THAT PROBABLY HAVE NO OR LITTLE EFFECT ON C DIFF INFECTION
 1. Antibiotic Eye Drops: Only a small amount of antibioitic is absorbed
1. Antibiotic Eye Drops: Only a small amount of antibioitic is absorbed
2. Topical Antibiotics: Only a small amount of antibioitic is absorbed
3. Ear Drops: Only a small amount of antibioitic is absorbed
4. Acetaminophen (Tylenol)
5. Chlorine and Florine in Drinking Water
 Neither Chlorine or Florine in the water have been well studied,
but one study found NO
significant changes in the gut microbiomes due to chlorine or florine.
There were some changes, but the changes were not considered
significant. There are no known studies on an association
between c diff and chlorinated or florinated water.
Neither Chlorine or Florine in the water have been well studied,
but one study found NO
significant changes in the gut microbiomes due to chlorine or florine.
There were some changes, but the changes were not considered
significant. There are no known studies on an association
between c diff and chlorinated or florinated water.
Reference: Chlorine and Florine
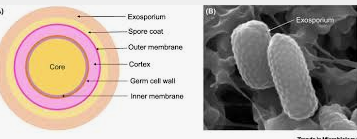 6. C Diff Spores in Food
6. C Diff Spores in Food
There are also numerous studies that have found c diff spores in the food we eat:
mainly meats, poultry, and fish, but also in some vegetables such as potatoes.
But, these studies do not include any studies that found that either animals
or people have became infected from eating food.
Thus, even though there
PROBABLY are some c diff spores in the foods we eat, it is NOT known if there is a
sufficient quantity of c diff spores in food to cause a new C diff infection.
The Canadian Goverment C Diff Fact Sheet states that if food is
cooked at 250 degrees F for 15-30 minutes
it will kill c diff bacteria AND SPORES.
Reference: No Food Transmission of C. diff.
Reference: What Kills C, diff.
Reference: Baking Food Probably Kills D diff Spores
3. Low-dose Over-The-Counter NSAIDS (Non-Steroidal Anti-Inflammatory Drugs)
 There is a study, which used
mice to examine an association between c diff and indomethacin
(which is a prescription strength NSAID)--BUT, other
researches have stated this Indomethecin study is flawed because
it failed to take into account treatment assignment bias.
In addition, this study only looked at the effect of Indomethacin, it did not
look at over-the-counter (OTC) NSAIDS,
such an ibuprofen, naprasyn, and aspirin.
There is a study, which used
mice to examine an association between c diff and indomethacin
(which is a prescription strength NSAID)--BUT, other
researches have stated this Indomethecin study is flawed because
it failed to take into account treatment assignment bias.
In addition, this study only looked at the effect of Indomethacin, it did not
look at over-the-counter (OTC) NSAIDS,
such an ibuprofen, naprasyn, and aspirin.
A retrospective study, looking at data from hospitalized patients,
who were taking OTC NSAIDS, like ibuprofen,
failed to find any association between OTC NSAIDS and c diff.
Thus, eventhough there is suggestive evidence
from the Indometheacin Mouse
study, there is no evidence confirming that OTC NSAIDs will have the same effect on humans.
The retrospective study
on humans found NO association between c diff and OTC NSAIDS.
Reference: OTC NSAIDS
IF YOU HAVE ANY QUESTIONS OR COMMENTS, PLEASE SEND THEM TO
DWIGHTTHOMASPARTNER@GMAIL.COM

XI. Ideas To Manage Anxiety
1. Consider WRITING your feelings down in a journal
2. Consider Therapy by a trained therapist
3. Consider Automatic Intelligence Therapy (AI Therapy)
A. Supposably Free: Ash AI Therapy, Earkick, and Wysa
B. Youper, Sanvello, Earkick, Serena, and more
4. Consider DISTRACTING yourself from WORRYING by any means possible:
A. Talk with friends: Not always about your health
B. Walk
C. Watch TV, Movies, Netflix, etc.
D. Play games
E. Read a good book silently or OUTLOUD
F. Work
5. Consider Medications
A. Ativan, Xanax, Valium
B. Atarax
C. Antidepressants (Zoloft, Celexa, Lexapro )
D. CBD
XII. Things to be Cautious About
1. It is important to manage c diff carefully because approximately 15-30,000
people die in the USA each year due c diff. In about 20 to 25% of people with a C. Diff. infection, C. Diff. returns.
These people will oftentimes require a repeat dose of either Dificid or Vancomycin—
or they may need a
prolonged course of Vancomycin or tapered Dificid, or even an FMT.
2. All medication and supplements, including probiotics,
antibiotics that treat C. Diff and FMTs, have a risk of side effects.
Sometimes, adverse reactions are mild, such as nausea or rash, but sometimes they can cause a more severe
reaction such as extreme diarrhea or an anaphylactic reaction, where a person is unable to breathe.
Probiotics and FMT's are also capable of causing various types of adverse reactions.
Therefore, everyone should be careful when trying a new medication or supplement.
If it is possible, it is best to start at a very low dose.
3. When a person has c diff, it is important to distinguish between diarrhea and mucus.
Low doses of Imodium or Lomotil and other anti-diarrheal medications can be used once a
person has been started on antibiotics; however, MUCUS will not respond to antidiarrheal medications.
And if a person takes anti-diarrheal medications for mucus, they might cause
constipation. Diarrhea usually consists of a high amount of watery discharge, whereas mucus
is generally a small amount of slippery discharge. Mucus in the colon is usually caused by
inflammation of the colon--but it is not diarrhea.
4. Drugs such as Imodium and Lomotil that decrease diarrhea might be detrimental in the
treatment of diarrhea caused by C. Diff. This is because C. Diff. bacteria make a toxin,
and if diarrhea is slowed down, this may leave the C. Diff Toxin in contact with a
patient's colon for a longer period of time. However, this has not been proven.
5. Medications such as creams, lotions, and gels should be tested in small dosages
in areas of the body that are not easily seen the first time they are used.
6.Consult “Epocrates.com
”
for each Specific Medication’s possible “Adverse Reactions.”
Side effects are also referred to as “ Adverse Reactions.”
Epocrates.com will tell you both “common reactions” and “serious
reactions.” You will have to create an account, but it is simple, fast, and free.
XIII. Success Stories

If anyone would like to tell their success story on how they successfully treated c diff
and have it published here or
in a book, please send it to me at dwightthomaspartner@gmail.com
Please follow the following format.
Name: (Fictitious or real)
Age:
Gender:
Where you grew up:
Where are you currently living:
Number in family:
Your profession:
Any other details you think would make an interesting story:
At what age did you get c diff:
What do you think was the cause of your first c diff illness:
How many times have you had c diff:
The different treatments you tried:
Any mistakes you made:
What treatment finally worked:
What is your advice for others who have c diff:
My Own Success Story (while waiting for others)
 Name: My name is Tom Partner and I’m 70 years old.
I grew up in Pittsburgh, PA. , but, I currently
live in Los Angeles, CA. I am single and don’t have any children.
I am a nurse practitioner, and I have been for the last 17 years.
Before that, I was a RN and a Health Teacher.
Name: My name is Tom Partner and I’m 70 years old.
I grew up in Pittsburgh, PA. , but, I currently
live in Los Angeles, CA. I am single and don’t have any children.
I am a nurse practitioner, and I have been for the last 17 years.
Before that, I was a RN and a Health Teacher.
About age 31, I had a small hemorrhoid surgery. I got a small infection from the surgery and was advised to take 7 days of Recephin IV, which I did. A week or two later, I had my first case of c diff. I was treated with 2 rounds of metronidazole and 1 round of vancomycin and finally got better.
For the next 30 years, I was good. However, I developed appendicitis at age 62 and had to have an appendectomy. I, of course, had to take antibiotics for the surgery, and again I got c diff. Since that time, I have had c diff 3 more times, usually following antibiotics, but one time there were no antibiotics. I probably had c diff 4 times between the ages of 62 and 68.
At age 68, following 3 courses of vancomycin, I got an FMT via colonoscopy. After 21 days and a change in diet to mostly rice, I had a normal bowel movement and have been relatively well since then.
Over the course of about 5 years, I tried over 10 different treatments for c diff. These included: metronidazole, vancomycin, Dificid, FMT, psychotherapy, a tiny amount of bentonite clay, nortriptyline (Pamelor), amitriptoline (Elavil), mirtazapine (Remeron), Pepto-Bismol, Imodium, cholestyramine (Questran), Welchol, sunbathing, Lotrimin cream, Vaseline, fasting, eating once a day, eating only bread and water, eating only rice and water.
The big mistake I made was listening to my primary care physician, who suggested I use Rocephin to treat a small infection that occurred as a result of hemorrhoid surgery. The infection was not that bad. I think I could have taken a less powerful antibiotic. I also tried amitriptyline (Elavil) and mirtazapine (Remeron). These are two antidepressants that can increase the chance of relapse, but I did not know that at the time. I also think I exercised too much, which I did not know at the time, that excess exercise can decrease a person’s immune system. Lastly, I thought maybe I could starve the c diff bacteria, so I tried fasting, but that did NOT help. It probably made it worse.
The treatment that finally worked was 3 courses of Vancomycin plus an FMT via colonoscopy. I had avoided an FMT for 4 years. But after 4 years, I decided to try it because I felt I no longer had much to lose. It seemed like my life was an endless loop of illness and moderate recovery, always watching what I was eating, and always worried that c diff would recur if I ate the wrong food, took an antibiotic, or exercised too much. Fortunately, the FMT treatment and trying to eat the right foods have worked for the last 2 years.
My advice for others is:
1. Read my website and some of the references listed
2. Learn from my and other people’s mistakes
3. Consider all possible treatments, BUT be cautious
4. Slowly and Carefully make adjustments to diet, medication, and exercise
 Name: My name is Tom Partner and I’m 70 years old.
I grew up in Pittsburgh, PA. , but, I currently
live in Los Angeles, CA. I am single and don’t have any children.
I am a nurse practitioner, and I have been for the last 17 years.
Before that, I was a RN and a Health Teacher.
Name: My name is Tom Partner and I’m 70 years old.
I grew up in Pittsburgh, PA. , but, I currently
live in Los Angeles, CA. I am single and don’t have any children.
I am a nurse practitioner, and I have been for the last 17 years.
Before that, I was a RN and a Health Teacher.
About age 31, I had a small hemorrhoid surgery. I got a small infection from the surgery and was advised to take 7 days of Recephin IV, which I did. A week or two later, I had my first case of c diff. I was treated with 2 rounds of metronidazole and 1 round of vancomycin and finally got better.
For the next 30 years, I was good. However, I developed appendicitis at age 62 and had to have an appendectomy. I, of course, had to take antibiotics for the surgery, and again I got c diff. Since that time, I have had c diff 3 more times, usually following antibiotics, but one time there were no antibiotics. I probably had c diff 4 times between the ages of 62 and 68.
At age 68, following 3 courses of vancomycin, I got an FMT via colonoscopy. After 21 days and a change in diet to mostly rice, I had a normal bowel movement and have been relatively well since then.
Over the course of about 5 years, I tried over 10 different treatments for c diff. These included: metronidazole, vancomycin, Dificid, FMT, psychotherapy, a tiny amount of bentonite clay, nortriptyline (Pamelor), amitriptoline (Elavil), mirtazapine (Remeron), Pepto-Bismol, Imodium, cholestyramine (Questran), Welchol, sunbathing, Lotrimin cream, Vaseline, fasting, eating once a day, eating only bread and water, eating only rice and water.
The big mistake I made was listening to my primary care physician, who suggested I use Rocephin to treat a small infection that occurred as a result of hemorrhoid surgery. The infection was not that bad. I think I could have taken a less powerful antibiotic. I also tried amitriptyline (Elavil) and mirtazapine (Remeron). These are two antidepressants that can increase the chance of relapse, but I did not know that at the time. I also think I exercised too much, which I did not know at the time, that excess exercise can decrease a person’s immune system. Lastly, I thought maybe I could starve the c diff bacteria, so I tried fasting, but that did NOT help. It probably made it worse.
The treatment that finally worked was 3 courses of Vancomycin plus an FMT via colonoscopy. I had avoided an FMT for 4 years. But after 4 years, I decided to try it because I felt I no longer had much to lose. It seemed like my life was an endless loop of illness and moderate recovery, always watching what I was eating, and always worried that c diff would recur if I ate the wrong food, took an antibiotic, or exercised too much. Fortunately, the FMT treatment and trying to eat the right foods have worked for the last 2 years.
My advice for others is:
1. Read my website and some of the references listed
2. Learn from my and other people’s mistakes
3. Consider all possible treatments, BUT be cautious
4. Slowly and Carefully make adjustments to diet, medication, and exercise
XIV. Frequently Asked Questions.
 If you earn less than $62,000/year, or you and your spouse make less than $84,000/year,
or your family of 4 earns less than $128,000/year, you MIGHT be eligible to obtain Dificid
for free, or for $50.
If you earn less than $62,000/year, or you and your spouse make less than $84,000/year,
or your family of 4 earns less than $128,000/year, you MIGHT be eligible to obtain Dificid
for free, or for $50.
Contact the Merck Pharmaceutical Company, the manufactures of Dificid (fidaxomycin).
Merck Contact Information
2. What do if I do if I have a positive C diff Toxin Test but I don't have symptoms?
 The general recommendations if you don't have symptoms of c diff
is NOT to take antibiotics. Taking any antiobiotics,
even Dificid and Vancomycin have some risk. You can continue to monitor yourself for symptoms and if
symptoms occur, you can either retest for c diff to make sure that is what you have or you can begin treatment for c diff.
The general recommendations if you don't have symptoms of c diff
is NOT to take antibiotics. Taking any antiobiotics,
even Dificid and Vancomycin have some risk. You can continue to monitor yourself for symptoms and if
symptoms occur, you can either retest for c diff to make sure that is what you have or you can begin treatment for c diff.
 There seems to be disagreement from different medical sources.
According to a UCLA (University of California Los Angeles) Website, the combination of Simethicone
and Activated Charcoal it the best solution for gas and bloating. However, another prestigious medical
website called UpToDate does NOT suggest the use of simethecone and activated charcoal.
A third medical site called American Family Physician, suggests either the use of Rifaximin
(which is a very expensive antibiotic usually used for SIBO), or or Probiotic supplements.
There seems to be disagreement from different medical sources.
According to a UCLA (University of California Los Angeles) Website, the combination of Simethicone
and Activated Charcoal it the best solution for gas and bloating. However, another prestigious medical
website called UpToDate does NOT suggest the use of simethecone and activated charcoal.
A third medical site called American Family Physician, suggests either the use of Rifaximin
(which is a very expensive antibiotic usually used for SIBO), or or Probiotic supplements.
Rifaximin +++ (The highest value of effect is ++++)
Probiotics
1. Prescript-Assist3 Volume +++
2. Bifidobacterium and Lactobacillus species mixtures +++ The use Alpha-galactosidase (Contained in Beano) can be of help if someone has flatus that is directly related to eating beans.
Reference: UCLA Website
Reference: American Association of Family Physicians
 The ideal treatment for constipation is to make an alteration in one's diet. For example,
to reduce rice and bread and increase fiber with vegetables and fruits. However,
if a diet change is insufficient then a person CAN look to medications. But, if there
is a chance of intestinal obstruction, a person should consult their doctor first before
taking oral medications for constipation. An intestinal obstruction CAN BE even worse than
having c diff.
The ideal treatment for constipation is to make an alteration in one's diet. For example,
to reduce rice and bread and increase fiber with vegetables and fruits. However,
if a diet change is insufficient then a person CAN look to medications. But, if there
is a chance of intestinal obstruction, a person should consult their doctor first before
taking oral medications for constipation. An intestinal obstruction CAN BE even worse than
having c diff.
If you fairly sure that your constipation is not due to an obstruction, you can consider any of the following:
1. Psyllium hust (Metamuciil)
2. Lactulose
3. Milk of Magnesia
4. Magnesium Citrate liquid
 None of these medications have a known association with c diff.
Psyllium Husk (Metamucil) and Lactulose MIGHT be of some benefit.
There is a very small amount of evidence that Psyllium Husk and Lactulose will NOT ONLY
help relieve constipation but will also reduce the rate of c diff relapse.
Magnesium is a well known laxative and is active ingredient in both Milk of Magnesia
and Magnesium Citrate.
There are no known studies associating Magnesium and the chance of c diff relapse.
None of these medications have a known association with c diff.
Psyllium Husk (Metamucil) and Lactulose MIGHT be of some benefit.
There is a very small amount of evidence that Psyllium Husk and Lactulose will NOT ONLY
help relieve constipation but will also reduce the rate of c diff relapse.
Magnesium is a well known laxative and is active ingredient in both Milk of Magnesia
and Magnesium Citrate.
There are no known studies associating Magnesium and the chance of c diff relapse.
Reference: Metamucil
Reference: Lactulose

In the northern hemispher the usual peak flu season is after Christmas, January and February. Therefore, often times, there is no rush to get the flu vaccination.
Also, it is important to remember that the flu vaccination is only effective about 40% of the time.
Other members of an infected person's family MIGHT want to be vaccinated to protect the infected person.
Even though there is no known association between the flu vaccination and c diff, this might be because it has never been studied.
*If a person is in a position where there is a high risk of getting the Flu, the risk and benefit of getting the Flu vaccinated must be recalculated.
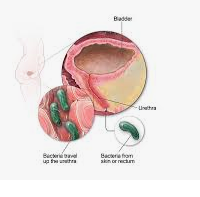
Urinary tract infection after having c diff is very concerning. There is no easy way to prevent URI
but there a couple of options.
Non-Antibiotic Medications:
1. Methenamine: This medication works by making the urine acidic, which inhibits bacterial growth.
2. D-Mannose supplement. It attaches to bacteria in the urine and prevents them from attaching
to the walls of the bladder.
3. Probiotics: specific strains of lactobacilli. Lactobacillus rhamnosus GR-1 and L. reuteri RC-14 (previously
called L. fermentum RC-14) seemed to be the most effective among the studied lactobacilli for
the prevention of UTIs. L. casei shirota and L. crispatus CTV-05 have also shown efficacy in some studies.
Reference: Probiotics for UTIs
Post-Menopausal Women might consider Vaginal estrogen. It changes the bacteria in
the vagina to reduce bad bacteria.
Small Doses of Antibiotic can be tried--If Other Measures are Ineffective
1. Macorbid (Nitrofurantoin)
2. Bactrim (Trimethoprim-sulfamethoxazole)
3. Fosfomycin

The standard treatment for a UTIs caused by E. Coli are the following:
Macrobid, Bactrim, Fosfomycin, and Keflex.
Of these, Macrobid is the least likely to cause a c diff relapse.
Non-conventional antibiotics that can be tried for UTIs due to E. Coli are:
Doxycycline, and Gentamycin IM.
These antibiotics are less likely to cause a c diff relapse.
Reference: Doxycycline
Reference: Gentamycin IM
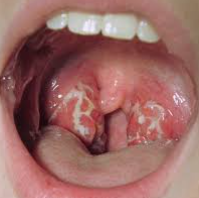
Penicillin V or Amoxicillin.
For people who are allergic to penicillin: Azithromycin, Chlarythromycin, and Clindamycin can be used.
A non-conventional treatment for strep throat is Doxycycline.
Doxycycline is less likely to cause a c diff relapse. However, although Doxycycline does kill some strains of Group A beta hemolytic streptococcal bacteria, some strains are resistive.
Reference: Doxycycline
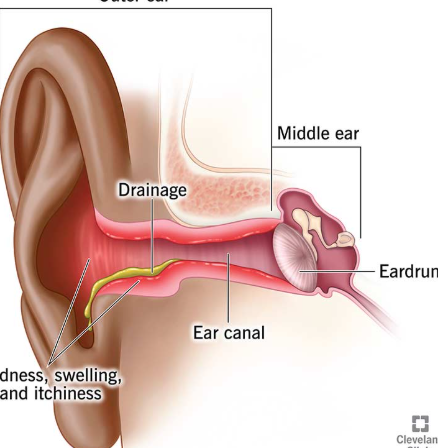
When a person has ear pain, it must be determined if the pain is coming from the middle ear
or the outer ear. Usually, if it is an outer ear infection, the person will have pain when
they touch
or move the outer ear. The outer ear infection, will usually only require antibiotic ear drops.
There is only a small amount of antibiotics in the ear drops and a small percentage of that
will be absorbed into the body. For these reasons, there is a low chance of causing c diff.
Commomn treatments for an outer ear infection (otitis externa) include the following:
Ciprofloxacin/dexamethasone, ofloxacin, and ciprofloxacin ear drops.
For severe ear infections oral antibiotics can be used. Ciprofloxacin, Amoxicillin, and
Augmentin are common medications recommended for severe otitis externa, but each of these
has a high risk of causing a c diff infection. (Epocrates.com) Among these Ciprofloxacin
probably has the lowest risk of causing c diff.
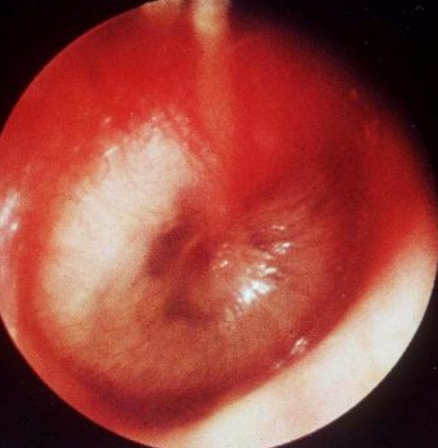
Augmentin, Amoxicillin, Omnicef (Cefdinir)
Azithromycin (if a person was allergic to penicillin).
Doxycycline, Clarithromycin, and Levofloxacin can also be used.
Of these, Doxycycline is considered the lowest risk of causing c diff; however, it is probably NOT the most effective.
Reference: Doxycycline Otitis Media: UpToDate
 Myringotomy and Tympanostomy:
Myringotomy and Tympanostomy:
A Non-coventional treatment, which is usually reserved for a child with repeated otitis media, is a myringotomy and tympanostomy. A myringotomy is a small surgical hole made in the tympanic membrane. A tympanostomy is a tube placed in the hole. The tube stays in place and if a person needs to have a treatment for an ear infection, he can be given antibiotic ear drops. These ear drops have a low risk of causing c diff. However, an ENT Doctor MIGHT NOT want to do this procedure because there are NO guidelines that suggest this procdeure should be used to prevent c diff infection.
Tympanostomy Video
Reference: Tympanostomy
Viral sinus infections are commonly mistaken for a bacterial sinus infection.
The best method of determining if a person has a bacterial or viral sinus
infection is to puncture the sinus and culture the specimen--but this is a
painful procedure and requires special training.
The second best method to determine
if a person has a bacterial sinus infection if to culture a mucus specimen
that is at the opening to the infected sinus. But, most doctors do NOT have an
endoscope; therefore, the best person to make a diagnois of a bacterial sinus infection
is an ENT doctor. But, even a culture does not guarantee the correct diagnosis.
The third way (and most common) to determine if a person has a bacterial
sinus infection is to examine the patients symptoms. The following are signs and symptoms
that can be examined.
1. Blood test: C-reactive protein: which becomes elevated when there is inflammation
2. White Blood Cell (WBC) Presence (this can be done with urine dipstick)
3. Thick mucus secretions
4. Pain in one sinus area
5. Temperature greater than 102 for three days
6. Symptoms greater than 10 days
7. One sided upper teeth pain
*. An on-line Calculator can also be used:
Bacterial Sinus Infection Risk Calculator
When it is possible an ENT doctor should examine a patient's sinus to determine
if that person has bacterial or a viral sinus infection or some other type of problem such
as a polyp or tumor.
The traditional antibiotics used for bacterial sinusitis are the following: Augmentin,
Clindamycin, Levofloxacin, and Doxycycline. Augmentin works the best is the most
likely to
cause a c diff relapse. Clindamycin is also has a very high risk of causing c diff.
Severe bacterial sinusitis
may require intravenous antibiotics.
Second Line Antibiotic:
Doxycycline is the least likely to cause a c diff infection--but
probably does work as well as the other antibiotics.
Common treatments for both streptococcal and staphyloccal bacteria Oral antibiotics including penicillin, clindamycin, erythromycin, cephadroxil (Duracef), Bactrim, and cephalexin (keflex). All of these have a risk of causing a c diff infection. Clindamycin is the most likely to cause a c diff infection.
Less Common Antibiotic for a Skin Infection:
Although doxycycline is used less commonly for skin infections, doxycycline has anti-bacterial qualities for all types of infections. It has anti-bacterial properties to not only staphylococcusl aureus and stretococcal pyrogenes, but also against MRSA. Therefore, although it is not considered a first-line treatment for a skin infection, it MIGHT be a good option for a person who is at a high risk for getting a c diff infection. Doxycycline is one of the lowest risk antibiotics for causing c diff.
Topical antibiotics such as mupiricin (Bactroban) is also effective in treating both streptococcal and staphylococcal skin infection. In addition, because very little is absorbed into the blood stream there is no known association with c diff.
If a person is thought to have a severe infection, they might need an intravenous medication such as vancomycin or linezolid.
This information is for the treatment of a MILD lung infection only.
If someone is having difficulty breathing. That person needs to go
to the Emergency Room for evaluation and treatment. This website will
not discuss the treatment for this type of lung infection. However,
mild to moderate lung infections can be discussed.
For the purpose of this discussion, let's talk about someone who either
been diagnosed with either bronchitis or a mild pnemonia.
Acute Bronchitis
(a recently occurring bronchitis) rarely starts
out as a bacterial infection, but it can
develop into one, especially if patients are over 80 years old or
over 65 with another serious illness. If there is no indication of a
bacterial infection, an inhaler such as Albuterol inhaler can relieve some symptoms
of bronchitis and there is no known association between Albuterol and c diff.
The antibiotics that are commonly ordered (if bacteria is suspected) is Azithromycin
and clarithromcyin. These are both a medium risk of causing a c diff infection.
Less Common Treatment for Bacterial Bronchitis.
Doxycycline has been used for bacterial bronchitis and found to be
relatively effective. It is also one of the antibiotics with
a low risk of causing a c diff infection.
Reference: Doxycycline For Bronchitis
Mild Pneumonia
can also be treated with oral antibiotics most of the time.
There are nine different bacteria that cause pnemonia. The most common are
streptococcal, hemophilus influenza, and mycoplasm bacteria.
When are started it is usually impossible to know which type of baceria is
causing the infection. Therefore, the usual treatments for ADULTS with
pnemonia are usually Amoxicillin, Augemtin (amoxicillin and clavulanate)
Azithromycin, or Clarithromycin. Augmentin and Amoxicillin both have
a high risk of causing c diff. Azithromycin and Clarithromycin have a medium risk of causing
a c diff infection.
Less Commonly Used: Doxycycline
Although Doxycycline is not USUALLY used as often as other antibiotics for
pnemonia it can be used and it has a much less chance of causing a c diff
infection.
Reference: Doxycycline for
Pnemonia

1. A few seconds before having a bowel movement, apply a barrier to anal area (Vaseline, A&D ointment, etc.)
2. Wash the anal area with mild water and soap. Some people find a bidet wash to be helpful. If time permits, a shower is probably the best way to keep the anal area clean.
3. Pat dry the anal area. A hair dryer on low heat can be used. Do NOT rub the area roughly.
4. Consider applying OTC Hydrocortisone or Lotrimin cream to the anal area
5. Lidocaine gel 4% (OTC) can also be applied for severe pain.
6. If hemorrhoids are present and extend outward, they should be gently pushed back in.
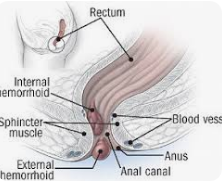 Sometimes, when people have excessive bowel movements they will develop
hemorrhoids. A hemorrhoids is basically a vein in the anal area that has
ballooned out.
Sometimes, when people have excessive bowel movements they will develop
hemorrhoids. A hemorrhoids is basically a vein in the anal area that has
ballooned out.
1. The First and Most important treatment for hemorrhoids
is to avoid straining. When a person has c diff, they
may experience a feeling that their is something in their
rectum, this is called tenesmus. This feeling may increase their
desire to push, or bear down. This MUST be avoided, in
order to avoid getting hemorrhoids or to treat hemorrhoids.
2. A few seconds before having a BM, a person should apply a barrier skin
to their anal area.
(Vaseline, A&D ointment, etc.)
3. After having a bowel movement, wash the anal area with mild water and soap.
Some people find
a bidet wash to be helpful. If time permits, a shower is
probably the best way to keep the anal area clean.
4. Pat dry the anal area. Do NOT rub the area roughly.
A hair dryer on low heat can be used.

5. Apply OTC Hydrocortisone or Lotrimin cream to the anal area
6. Lidocaine gel 4% (OTC) can also be applied for severe pain
7. If hemorrhoid are external, they should
be gently pushed back in.
8. Sometimes hydrocortisone suppositories can help. This is usually placed
in the rectum before a person goes to sleep. The hydrocortisone
can reduce inflammation inside the rectum.
9. If someone has very severe hemorrhoids, a more invasive
treatment MIGHT be needed. (Usually, hemorrhoids will shrink to normal
if they are not stressed for a period of time.) However, if
hemorrhoids are unsuccessfully treated with the above mentioned
treatments, there are other treatments. These treatments include
rubber band ligation, sclerotherapy, coagulation therapy and surgery.
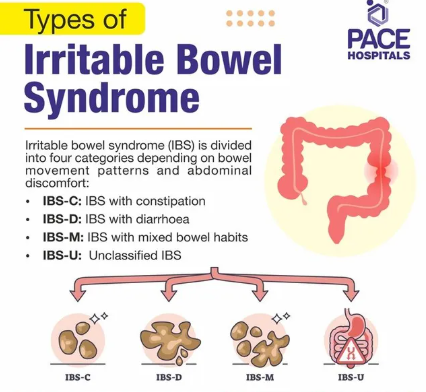
The most conservative treatment for PI-IBS is a change in diet. If someone has IBS-C (constipation), high-fiber foods are recommended. If someone has IBS-D (diarrhea), low-fiber foods are recommended. This is essentially the same as a low-FODMAP diet. FODMAP stands for fermentable oligosacharides, disacharides, monosaccharides, and polyols. These are foods that are harder to digest. Examples are the following:
Vegetables: Garlic, onions, leeks, broccoli, cauliflower, and mushrooms.
Fruits: Apples, pears, mangoes, cherries, and dried fruits.
Dairy: Cow's milk, soft cheeses, ice cream, and yogurts.
Grains and cereals: Wheat, rye, and barley products, and many breakfast cereals.
Legumes and nuts: black beans, kidney beans,lentils, cashews and pistachios.
If people continue to have loose stools and diarrhea despite eating a low-fiber diet they can try an elimination diet. There is several ways an elimination diet can be done.
 One way to try an elimination diet is to avoid foods or drinks that a person suspects
is causing them diarrhea. The second way is to start with very basic foods
such as white rice and water and then slowly test one ADDITIONAL NEW
food at a time for a
day or two to see if they can tolerate that food. If a food is tolerated
it remains in the diet, if a food is not tolerated it is eliminated--but, can
be retried in a month or two.
If changing the diet
does not work, then a person can try medications.
One way to try an elimination diet is to avoid foods or drinks that a person suspects
is causing them diarrhea. The second way is to start with very basic foods
such as white rice and water and then slowly test one ADDITIONAL NEW
food at a time for a
day or two to see if they can tolerate that food. If a food is tolerated
it remains in the diet, if a food is not tolerated it is eliminated--but, can
be retried in a month or two.
If changing the diet
does not work, then a person can try medications.
The most common medication for IBS (diarrhea) are the following: cholestyramine (Questran), loperamide (Imodium), dicyclomine (Bentyl), nortriptoline (Pamelor), amitriptoline, paroxetine (Paxil), (Elavil), hyoscyomine (Levsin),
Reference: Epocrates.com
 A couple of these have less potential side effects than the others. Dicyclomine,
cholestyramine, and loperamide have less possible side effects.
Antidepressants such as nortriptoline, amitriptoline,
and paroxetine have more side effects and
MIGHT increase the chance of c diff relapse. According to one study,
paroxetine and
amitriptoline have a about a two-fold risk or increasing relapse--
but nortriptoline MIGHT increase the risk of
c diff infection as much as four times. (However, some studies found NO
Increased Risk with these antidepressants.)
A couple of these have less potential side effects than the others. Dicyclomine,
cholestyramine, and loperamide have less possible side effects.
Antidepressants such as nortriptoline, amitriptoline,
and paroxetine have more side effects and
MIGHT increase the chance of c diff relapse. According to one study,
paroxetine and
amitriptoline have a about a two-fold risk or increasing relapse--
but nortriptoline MIGHT increase the risk of
c diff infection as much as four times. (However, some studies found NO
Increased Risk with these antidepressants.)
Reference: SOME Antidepressant MIGHT Increase the Risk of C. diff.
If a person has IBS-c (constipation). there are several medications that can be tried Metamucil, Lactulose, Miralax, Milk of Magnesia, Magnesium Citrate, and Senokot. Metamucil, Lactulose, and Miralax are probably the safest.

Provided that the cause of a person's nausea
is known (for example c diff) a person can usually be treated
with common medications for nausea.
The most commonly used medication for nausea are odansetran (Zofran),
promethazine (Phenergan), metoclopramide (Reglan), and
prochlorperazine (Compazine). Of these, odansetran is the most
commonly used. Odansetran works by blocking the NAUSEA nerve receptor.
Reference: Common Medications for Nausea
There is one other medication that can be considered for nausea that
does not respond to odansetran, and that is gabapentin (Neurontin).
Neurontin works by slowing nerve transmissions down, and c diff
can sometimes overstimulate nerves.
Reference: Gabapentin Anti-Nausea
18. What is the best treatment for Intestinal Cramps?
Reference: Antispasmodic Medications Mayo Clinic>
Reference: AJG Review of Antispasmodics
The two most commonly used in the United States are dicyclomine (Bentyl) and hyoscyamine (Levsin). There is no known association with the use of these medications and increased risk of c diff; however, they do tend to slow down gastric motility and excessive use MIGHT theoretically increase the chance of a c diff relapse.

The Center Disease Control (CDC) states that a person can return
to work 2 days after their symptoms stop.
Per CDC: "You should only resume everyday life
(return to work or school) after symptoms stop."
However, this information
is ambiguous because the term "symptoms" is ambiguous. Which symptoms
are the CDC talking about, loose stools, fatigue, fever, abdominal pain.
Some people will require months before all of their symptoms stop.
Therefore,
the CDC's guideline is Not very useful.
Reference: CDC's Guidelines for Returning
to Work
There are NO EXACT criteria as to when to return to work.
The logical answer is that a person can return to work when they
feel almost normal. But, c diff has about a 25% chance of relapse and
many people have PI-IBS for months to years after having c diff.
Therefore, these additional facts make it almost impossible
to say when a person can or should return to work. It is basically
up to the individual and their doctor to decide when they should
return to work.

Reference: Exercise Can be both Good or Bad
1 of 7 Marathon Runners Get Sick Reference

Generally speaking, your family will be protected from
getting c diff by their own good intestinal bacteria.
Many people who are well have c diff spores in their
intestines and these spores never germinate (grow into active
infections) because good gut bacteria inhibit them from growing.
To further reduce the risk of transmission of c diff
to other family members it is
important to try to limit the number of c diff spores. C diff
spores can never be totally elminated because they are everywhere,
with the fast majority being on the ground.
Of course a person who has an active infection will not only have
some spores but will also have some active bacteria. The active
c diff bacteria will die by themselves when exposed to air for
a couple of hours. The c diff SPORES require either a solution containing
sodium hypochlorite or hydrogen peroxide. Sodium hypochlorite is found
in bleach. It can also be found in cleaning wipes. A person can
make their own cleaning solution with one part bleach and 9 parts water.
If hydrogen peroxide is used, it should be a 7% solution or higher.
The over-the-counter hydrogen peroxide perparations
only contains 3-6%; therefore, they are not recommended for cleaning.
It is important to note that once a hard surface is wiped with a
sodium hypochlorite solution, it should be left on the surface for
5-10 minutes to be effective. Also, sodium hypochlorite will bleach the
color out of fabric so therefore it can only be used on hard surfaces.
There is no practical way to clean carpets and fabric furniture.
Wearing disposable latex gloves and good handwashing
can further
reduce the chance of c diff transmission.
Reference: Cleaning Supplies for C. diff.
